What to do About Rising Health Care Costs?
 Speakers at the 2017 annual meeting of the Academy of Managed Care Pharmacy took on rising health-care costs. In a presentation, Steven G. Avey, RPh, MS, FAMCP, Vice President of Specialty Clinical Programs and Michael Ciarametaro, MBA, Vice President of Research at the National Pharmaceutical Council, spoke on the issue and its effects on pharmacy.
Speakers at the 2017 annual meeting of the Academy of Managed Care Pharmacy took on rising health-care costs. In a presentation, Steven G. Avey, RPh, MS, FAMCP, Vice President of Specialty Clinical Programs and Michael Ciarametaro, MBA, Vice President of Research at the National Pharmaceutical Council, spoke on the issue and its effects on pharmacy.
A major problem for patients and the health-care system—how higher-than-anticipated drug prices and patients who are stuck with more of the cost burden means more nonadherence and waste. For nonspecialty drugs, patient copays represent 20% to 25% of the drug’s cost, but for specialty drugs, copays represent less than 2% of the medication’s total cost. Avey was surprised, however, to see that financial concerns only represented 2% of patient responses in a patient survey.
The number one thing payers can do, Avey said, is to avoid waste, by addressing poor adherence, paying for the wrong dosage, gaps in care or inappropriate dosing, and prescribing drugs that are not indicated for the patient’s genetic mutation status. To prevent waste, he stressed that it is important for the specialty pharmacy to contact the provider and ask why a patient is not receiving or taking the appropriate regimen.
Ciarametaro discussed affordability, which is different for each stakeholder in the health-care system (patients, payers, society, or purchaser). He also made the distinction between affordability, value, and budget impact. “I would argue that increasing drug spending is not necessarily a negative indicator. We still need to figure out how much we should spend on drugs,” he said.
PBMs only have limited tools to deal with costs and interact with the various stakeholders, and they must deal with and balance covered therapies, utilization management, patient out-of-pocket costs, and rebate contracting with regard to premiums. A single determination of value is not adequate and needs to be tailored to the population, the condition, and the region of care, he said.
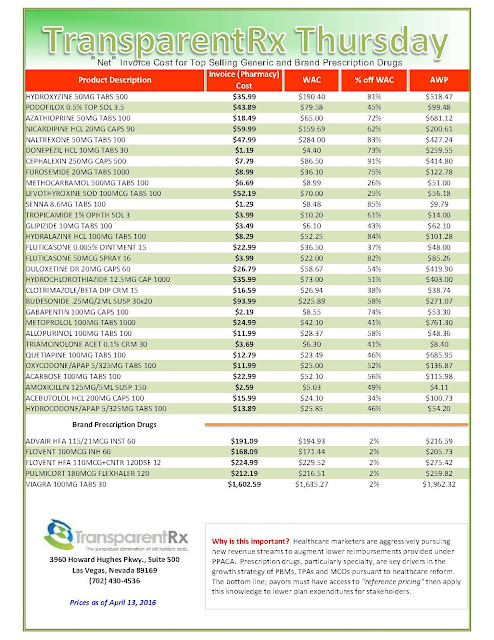
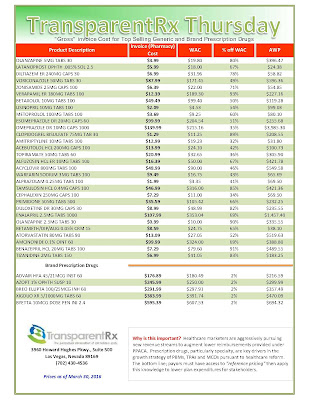
Reference Pricing: “Gross” Invoice Cost for Popular Generic and Brand Prescription Drugs (Volume 162)
The costs shared here are what the pharmacy actually pays; not AWP, MAC or WAC. The bottom line; payers must have access to actual acquisition costs or AAC. Apply this knowledge to hold PBMs accountable and lower plan expenditures for stakeholders.
Step #1: Obtain a price list for generic prescription drugs from your broker, TPA, ASO or PBM every month.
Step #2: In addition, request an electronic copy of all your prescription transactions (claims) for the billing cycle which coincides with the date of your price list.
Step #3: Compare approximately 10 to 20 prescription claims against the price list to confirm contract agreement. It’s impractical to verify all claims, but 10 is a sample size large enough to extract some good assumptions.
Step #4: Now take it one step further. Check what your organization has paid, for prescription drugs, against our acquisition costs then determine if a problem exists. When there is a 5% or more price differential (paid versus actual cost) we consider this a problem.
Multiple price differential discoveries means that your organization or client is likely overpaying. REPEAT these steps once per month.
— Tip —
Always include a semi-annual market check in your PBM contract language. Market checks provide each payer the ability, during the contract, to determine if better pricing is available in the marketplace compared to what the client is currently receiving.
When better pricing is discovered the contract language should stipulate the client be indemnified. Do not allow the PBM to limit the market check language to a similar size client, benefit design and/or drug utilization. In this case, the market check language is effectually meaningless.
New Solutions for Curbing Runaway Drug Costs
 |
| Click to Learn More |
The challenges associated with specialty pharmacy, biologics, and biosimilars require a whole new playbook, one with collaboration as the organizing principle. Payers and providers can work together in several areas to rein in the galloping drug spend:
- Clinical management. Given the rapid evolution of the pharmaceutical market, the question is no longer whether a treatment exists for a condition, but how effective it is. The pace of innovation and approvals puts a premium on keeping up with the incoming waves of new research, driving adherence to evidence-based protocols, and engaging with patients so they follow treatment as prescribed.
- Cost containment. When it comes to pharmaceutical cost and trend, misaligned incentives can get in the way of optimal solutions. Payers and providers must streamline their processes, especially as they pertain to medications, and wring out unnecessary expenditures whenever possible. Reducing costs can involve many levers, including standardizing therapies and negotiating prices accordingly, expanding the use of generics, exploring biosimilar alternatives, and optimizing use of the 340b program.
- Appropriate sites of care. When it comes to specialty drugs, the driver of total cost is not just in the unit pricing but also in how and where those drugs are administered. Costs can vary widely depending on whether a drug is administered in the physician office, at a specialty pharmacy, or at home. Working jointly to steer patients to the most effective sites will boost total effectiveness and help control costs.
None of this will be easy. Even if drug-cost legislation is enacted, there is no guarantee such controls will be effective absent providers and payers working together. But, if we can get it right, we can hold specialty pharmaceuticals to the same standards of value that are reshaping the rest of health care.
by Zachary Hafner
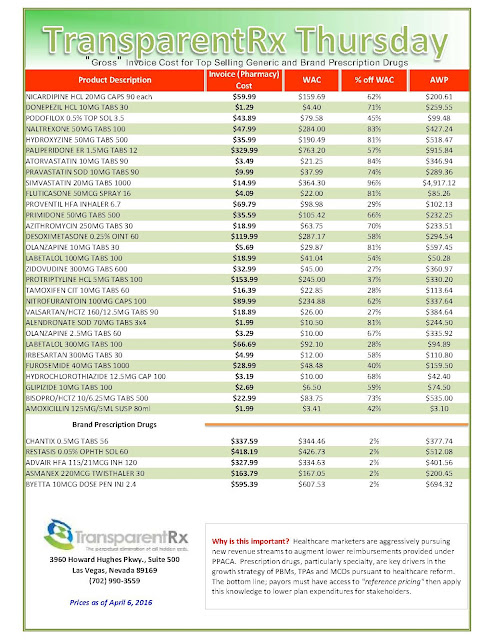
Reference Pricing: “Gross” Invoice Cost for Popular Generic and Brand Prescription Drugs (Volume 161)
The costs shared here are what the pharmacy actually pays; not AWP, MAC or WAC. The bottom line; payers must have access to actual acquisition costs or AAC. Apply this knowledge to hold PBMs accountable and lower plan expenditures for stakeholders.
Step #1: Obtain a price list for generic prescription drugs from your broker, TPA, ASO or PBM every month.
Step #2: In addition, request an electronic copy of all your prescription transactions (claims) for the billing cycle which coincides with the date of your price list.
Step #3: Compare approximately 10 to 20 prescription claims against the price list to confirm contract agreement. It’s impractical to verify all claims, but 10 is a sample size large enough to extract some good assumptions.
Step #4: Now take it one step further. Check what your organization has paid, for prescription drugs, against our acquisition costs then determine if a problem exists. When there is a 5% or more price differential (paid versus actual cost) we consider this a problem.
Multiple price differential discoveries means that your organization or client is likely overpaying. REPEAT these steps once per month.
— Tip —
Always include a semi-annual market check in your PBM contract language. Market checks provide each payer the ability, during the contract, to determine if better pricing is available in the marketplace compared to what the client is currently receiving.
When better pricing is discovered the contract language should stipulate the client be indemnified. Do not allow the PBM to limit the market check language to a similar size client, benefit design and/or drug utilization. In this case, the market check language is effectually meaningless.
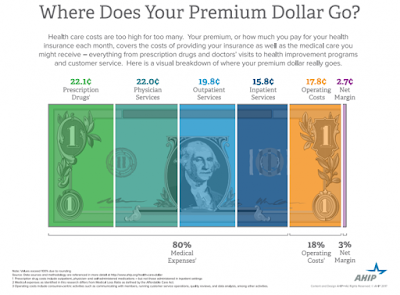
Prescription Drugs Account for 22% of Payer Premium Spending
Eighty percent of every dollar is spent on medical expenses, and the remaining 20 percent was split between operating costs and net margins, showing that payers are adhering to the 80/20 rule instituted by the ACA.
“This is the latest evidence that shows prescription drug costs are out of control,” said Marilyn Tavenner, President and CEO of AHIP in an accompanying statement.
 |
| Click to Learn More |
“The vast majority of every dollar spent by consumers on insurance premiums is returned in direct medical services, including prescription drugs. That’s why we need real solutions that answer the President’s call to ‘bring down the artificially high price of drugs’ so that consumers can affordably get the care they need.”
The AHIP report used data from premiums contributed by patients under 65 who were continuously insured.
Outpatient services consumed 19.8 cents of every dollar while 15.8 cents were spent on covering inpatient services. Operating costs for payers were 17.8 cents per premium dollar.
In 2014, healthcare expenses totaled $104 billion. Prescription drug spending accounted for $28.9 billion and physician services accounted for $28.8 billion. Outpatient and inpatient services, respectively, cost $26.1 and $20.7 billion.
“Don’t Miss” Webinar: How to Slash PBM Service Costs, up to 50%, Without Changing Vendors or Benefit Levels
Here is what some participants have said about the webinar.
“…Great presentation! I had our two partners on the presentation as well. Very informative.” Nolan Waterfall, Agent/Benefits Specialist
A snapshot of what you will learn during this 30 minute webinar:
- Hidden cash flows in the PBM Industry such as formulary steering, rebate masking and differential pricing
- How to calculate cost of pharmacy benefit manager services or CPBMS
- Specialty pharmacy cost-containment strategies
- The financial impact of actual acquisition cost (AAC) vs. effective acquisition cost (EAC)
- Why mail-order and preferred pharmacy networks may not be the great deal you were sold
Tyrone D. Squires, MBA
TransparentRx
2850 W Horizon Ridge Pkwy., Suite 200
Henderson, NV 89052
866-499-1940 Ext. 201
P.S. Yes, it’s recorded. I know you’re busy … so register now and we’ll send you the link to the session recording as soon as it’s ready.
Out-of-pocket costs based on drug list prices; a hidden fee
 |
| List Price vs. Actual Cost |
That’s according to new analysis from Amundsen Consulting, a division of QuintilesIMS, which found in spite of “robust negotiations between biopharmaceutical companies and payers,” health plans don’t pass along the savings achieved via rebates and discounts on the price of medicines, but instead still require patients with high deductibles or coinsurance to pay up based on the medications’ full list price.
“While biopharmaceutical companies set the list prices for their medicines, it is the health plan that ultimately determines how much a patient pays out-of-pocket,” Stephen J. Ubl, president and chief executive officer of the Pharmaceutical Research and Manufacturers of America (PhRMA), the organization that commissioned the analysis, says in a statement.
Ubl adds, “Even though more than a third of the list price is rebated back to payers and the supply chain, health plans do not pass along these discounts to patients with high deductibles and coinsurance.”
That often results in patients with high deductibles or coinsurance being more likely to stop taking medications as prescribed or even abandoning their prescriptions at the pharmacy. That in turn can expose them to higher risk for trips to the emergency room, otherwise avoidable hospitalizations and resulting poorer health.
According to a report in The American Prospect, the problem is pharmacy benefit managers, who act as middlemen in managing prescription drug benefits for health plans, “contracting with drug manufacturers and pharmacies in a multi-sided market.”
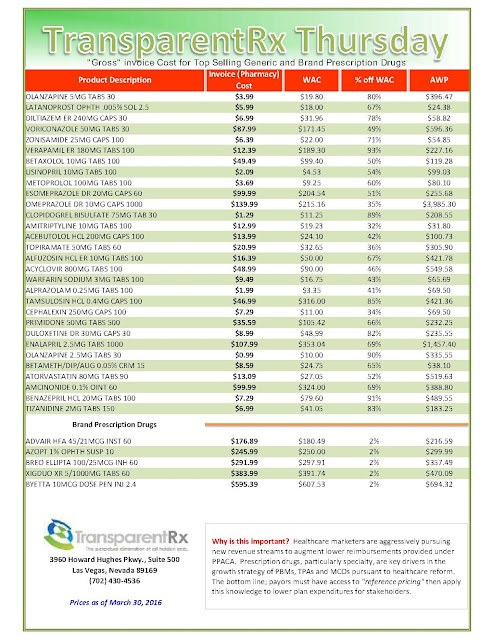
Reference Pricing: “Gross” Invoice Cost for Popular Generic and Brand Prescription Drugs (Volume 160)
The costs shared here are what the pharmacy actually pays; not AWP, MAC or WAC. The bottom line; payers must have access to actual acquisition costs or AAC. Apply this knowledge to hold PBMs accountable and lower plan expenditures for stakeholders.
Step #1: Obtain a price list for generic prescription drugs from your broker, TPA, ASO or PBM every month.
Step #2: In addition, request an electronic copy of all your prescription transactions (claims) for the billing cycle which coincides with the date of your price list.
Step #3: Compare approximately 10 to 20 prescription claims against the price list to confirm contract agreement. It’s impractical to verify all claims, but 10 is a sample size large enough to extract some good assumptions.
Step #4: Now take it one step further. Check what your organization has paid, for prescription drugs, against our acquisition costs then determine if a problem exists. When there is a 5% or more price differential (paid versus actual cost) we consider this a problem.
Multiple price differential discoveries means that your organization or client is likely overpaying. REPEAT these steps once per month.
— Tip —
Always include a semi-annual market check in your PBM contract language. Market checks provide each payer the ability, during the contract, to determine if better pricing is available in the marketplace compared to what the client is currently receiving.
When better pricing is discovered the contract language should stipulate the client be indemnified. Do not allow the PBM to limit the market check language to a similar size client, benefit design and/or drug utilization. In this case, the market check language is effectually meaningless.
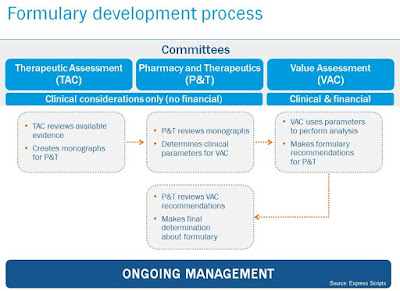
How do insurance companies decide what medicines to pay for and when to pay for them?
 |
| Click to Learn More |
Insurers and other payers look first at how well the drug works — not its cost — when they decide whether to cover the latest treatments, according to the nation’s largest pharmacy benefits manager, Express Scripts.
The price patients eventually pay gets determined later, when an insurance company or pharmacy benefits manager decides where a drug fits on a list of covered treatments called a formulary.
The cost of prescription drugs has become a growing source of concern with doctors and patients, but it’s not a factor considered by an independent committee used by Express Script to determine coverage of a new drug, Chief Medical Officer Dr. Steve Miller said.
That committee — 15 doctors and a pharmacist — reviews the information that federal regulators used to approve a drug and then decides whether it should be covered.
Some payer coverage decisions come with qualifications like a requirement that patients meet specific criteria or try other treatments first. That can limit patient access. Doctors say some patients have had trouble getting a new cholesterol-lowering drug, Repatha, that costs $14,000 a year, because of the restrictions.
Insurers largely use pharmacy benefits managers to set up the lists that determine how much a patient ends up paying. Some lists are divided into tiers, with drugs on the bottom generally being generic or least expensive. Those on the highest tier might include specialty medicines that could cost the patient hundreds of dollars even with coverage.
Whether a drug even gets on the list can depend on whether a similar medicine is already in the market. When the ground-breaking hepatitis C treatments Sovaldi and Harvoni from Gilead Sciences debuted a few years ago, Express Scripts had to include them. They cost more than $80,000 for a course of treatment, but the drugs essentially cure a debilitating disease and they had no competition.
But once the drugmaker AbbVie produced a third option, Viekira Pak, with a similar cure rate, Express Scripts was able to negotiate a price discount and switched to covering only Viekira Pak.
The nation’s two largest pharmacy benefits managers, Express Scripts and CVS Health Corp., both say they cover Repatha.
By Tom Murphy
- Go to the previous page
- 1
- …
- 91
- 92
- 93
- 94
- 95
- 96
- 97
- …
- 139
- Go to the next page