Drugmakers circumvent health plan sponsors’ benefit designs at the switch to have expensive brand pharmaceuticals dispensed. Why don’t decision-makers protest this more? By delivering eVouchers, or electronic vouchers, for pricey prescriptions at the “Switch,” brand drugmakers are getting past pharmacy coverage plan designs. The switch determines which PBM, or health plan, is to receive the third-party prescription claim and is linked to the drug. In a matter of seconds, the prescription leaves the pharmacy, makes its way to the switch, and is then sent to the PBM.
When the benefit design incorporates inadequate UM or utilization management restrictions, such as mandatory generic enforcement or step therapy drugmakers can use eVouchers to replace a tier 1 drug with a tier 2-4 drug or, worse yet, a non-formulary drug (see process flow diagram below). The two largest switch providers are Relay Health and Change Healthcare. Relay Health describes how its electronic voucher program is a Win-Win-Win resolution in the following way:
- Doctors “set aside concerns over costs”
- “Patients benefit from lower copays” and “increased adherence”
- Manufacturers benefit from increased “scripts written”, “the likelihood patients will fill and adhere to them” and “increased brand loyalty”
What about the health plan sponsor, though? Despite the fact that you pay most of the expenses, you are conveniently ignored. I demonstrate in our Certified Pharmacy Benefits Specialist (CPBS) course how plan sponsors, while knowing the least about how it operates, fund the whole US prescription drug system. Simply put, they are interested in your wallet. The switch operators’ eVoucher schemes have a huge budgetary impact on health plan sponsors, and that influence is only getting bigger over time.
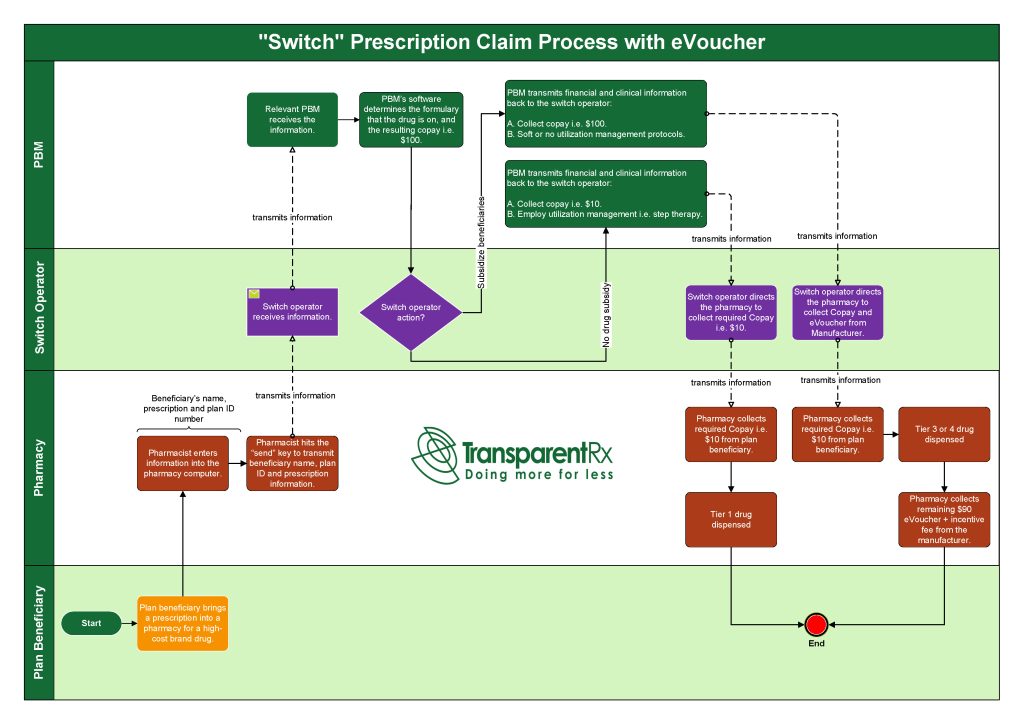
There are two ways to stop the scenario from occurring:
(1) PBM inserts a provision prohibiting the action into its contract with the Switch firm
(2) Benefit design maximizes the toolset for managing drug utilization, which includes mandatory generic enforcement programs, step therapy, refill to soon, and prior authorization just to name a few
Number two is challenging since many plan sponsors are adamant that employees receive the medications they desire without any restrictions (i.e. step therapy). Even though I disagree, it’s not my checkbook. The goal is to produce better health care outcomes at the lowest possible cost, not to save employees from the “discomfort” of managing an effective pharmacy benefit plan. In a way, pharmaceutical companies and non-fiduciary PBMs are taking advantage of HR’s desire to maintain employee “happiness.”
Drugmakers circumvent health plan sponsors’ benefit designs at the switch is a hidden cost. The decision for TransparentRx is straightforward: either you want an efficiently run pharmacy benefit program for your people or you don’t. Expect to spend $1,000 for a drug when, for instance, a $100 drug would have delivered the same degree of efficacy. eVouchers are an expensive proposition for health plan sponsors but a profitable one for brand drugmakers, especially when supplemented with direct-to-consumer TV commercials for expensive brand pharmaceuticals and soft utilization management measures.