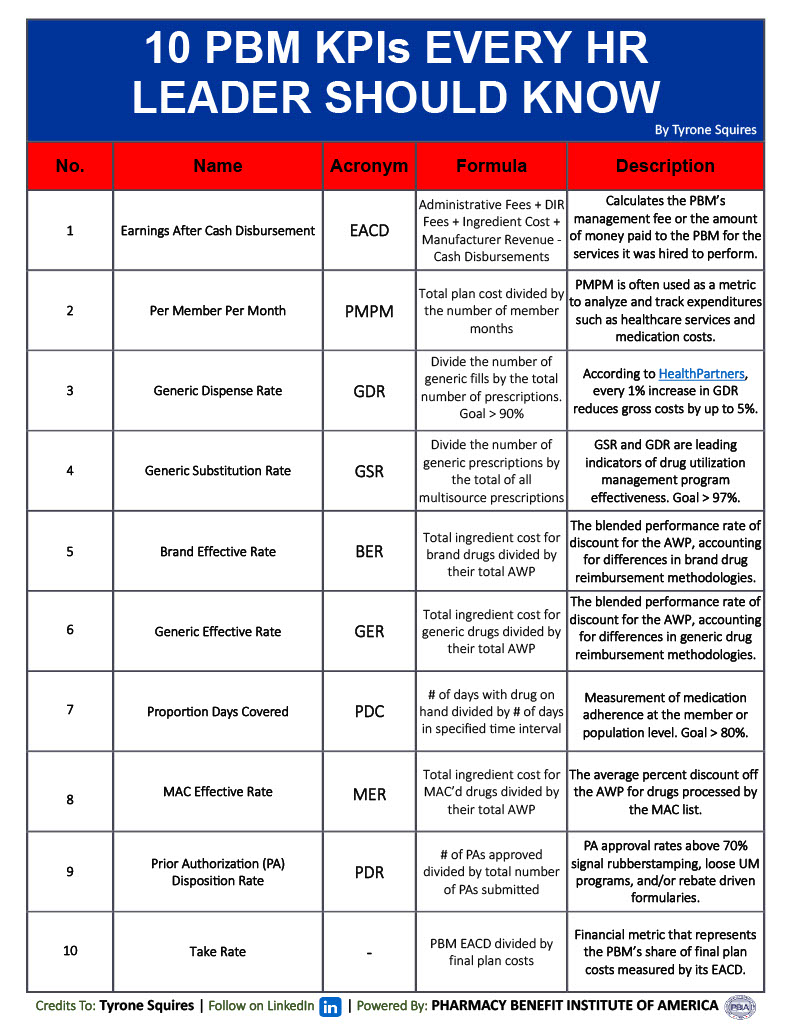
Understanding PBM Key Performance Indicators (KPIs) is crucial for HR and finance leaders. KPIs provide measurable and actionable insights into PBM performance, progress, and success. Furthermore, KPIs serve as quantifiable metrics that help assess the effectiveness and efficiency of PBM pricing and clinical programs. Mastering pharmacy benefit management (PBM) KPIs is crucial for the following reasons:
Performance Evaluation: KPIs provide a standardized and objective way to evaluate PBM performance at member, departmental, or organizational levels. By setting clear KPIs, HR and their consultants can monitor progress, identify strengths and weaknesses, and make data-driven decisions to improve performance.
Goal Setting and Alignment: KPIs play a crucial role in establishing SMART goals—specific, measurable, achievable, relevant, and time-bound. By offering a clear sense of direction, KPIs effectively channel efforts towards desired outcomes. When HR fully understands the KPIs, they can concentrate their actions and allocate resources to the areas of utmost importance, thereby facilitating the accomplishment of strategic objectives.
Decision Making: KPIs provide valuable insights that assist in making informed decisions. By tracking relevant KPIs, employee benefit brokers, consultants, and self-funded organizations gain visibility into what is working and what needs improvement. KPIs enable data-driven decision-making, helping to prioritize initiatives, allocate resources effectively, and adjust when required.
Continuous Performance Monitoring: KPIs serve as monitoring tools that allow individuals and organizations to track progress over time. Regularly reviewing KPIs helps identify trends, patterns, and areas of concern. By analyzing KPI data, organizations can identify bottlenecks, inefficiencies, or underperforming areas and take proactive measures to address them, leading to continuous improvement. Continuous performance monitoring is best done with software automation that doesn’t rely on PBM self-reporting.
Accountability and Transparency: KPIs promote accountability by clearly defining expectations and responsibilities. When KPIs are well-defined and understood, PBM and HR teams know what is expected of them. This fosters a sense of ownership and responsibility, leading to improved performance. Furthermore, transparently sharing KPI data within an organization promotes a culture of transparency, enhances communication, and enables collaboration.
Benchmarking and Performance Comparison: KPIs facilitate benchmarking by allowing organizations to compare their performance against industry standards, competitors, or their own historical data. Benchmarking helps identify areas where an organization is lagging or excelling, providing insights for improvement or potential areas of competitive advantage.
Communication and Stakeholder Management: KPIs provide a common language for communicating performance to stakeholders, whether they are employees, management, investors, or customers. Clear and well-defined PBM KPIs help stakeholders understand the progress, achievements, and challenges faced by an organization, fostering trust, and facilitating effective communication.
To ensure a successful relationship with their Pharmacy Benefit Manager (PBM), the self-insured organization and their advisors must possess a comprehensive understanding of their objectives and the competitive landscape. Additionally, they should be capable of compelling the PBM to provide pertinent information about essential services. Evaluating PBM transparency is best accomplished by a trained individual who possesses intimate knowledge of the buyer’s desired benefits and disclosure objectives. Pharmacy Benefit Managers will offer openness and disclosure to the extent that the competitive market requires them to do so, and they often depend on demands for information from potential customers when negotiating their contracts.
In summary, understanding PBM Key Performance Indicators (KPIs) is essential for individuals and organizations to monitor performance, set goals, make informed decisions, foster accountability, and drive continuous improvement. By leveraging KPIs effectively, self-insured organizations can enhance their competitiveness, achieve their objectives, and adapt to the ever-changing pharmacy benefit management landscape.