Winning Strategies for Plan Sponsors to Reduce Medical Benefit Drug Costs
Medical specialty drugs are among the fastest-growing cost drivers in healthcare, demanding a more strategic approach to reimbursement. Without proper oversight, self-funded employers and plan sponsors can overpay for these high-cost therapies, leading to unnecessary financial strain. Optimizing medical specialty reimbursement presents significant opportunities for plan sponsors to reduce medical benefit drug costs while maintaining clinical effectiveness.
Clinical Effectiveness
Ensuring clinical effectiveness means aligning medical specialty drug reimbursement with evidence-based protocols. This requires a framework that prioritizes therapies with proven outcomes and avoids unnecessary utilization. Establishing clinical guidelines and enforcing prior authorization policies can help curb waste while ensuring patients receive the right medication at the right time.
Pricing Validation: Paid vs. Billed
A frequent source of waste in specialty drug reimbursement is the gap between what is billed and what is ultimately paid. Providers may bill significantly higher amounts than negotiated contract rates, leaving employers at risk of overpayment. Rigorous auditing of claims and automated pricing validation tools can help identify discrepancies and ensure plan sponsors pay only what is contractually obligated.
Pricing Validation: Paid vs. Contract
Beyond billed versus paid amounts, discrepancies also exist between what is paid and the contracted rate with manufacturers, PBMs, or other intermediaries. Implementing real-time pricing validation tools ensures that payments adhere to contract terms, reducing financial leakage and preventing unnecessary markups. Employers should demand transparency from their vendors and hold them accountable for contract compliance.
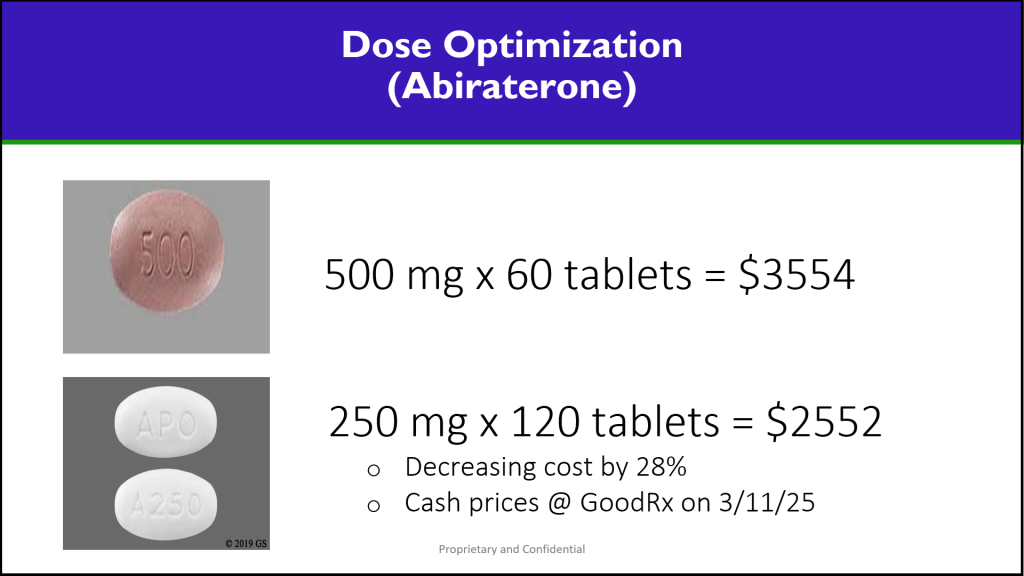
Dose Optimization
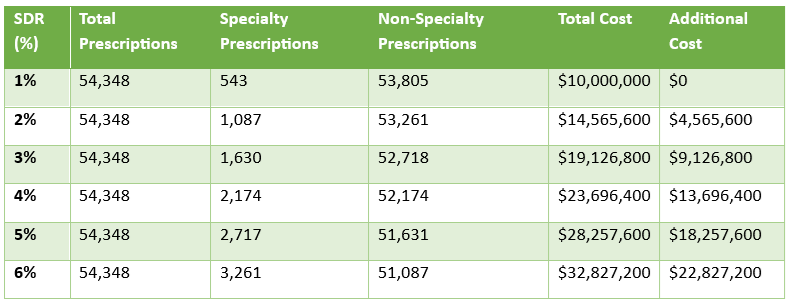
One of the most overlooked opportunities in medical specialty reimbursement is dose optimization. Many specialty drugs have flexible dosing options, yet providers often prescribe in a manner that maximizes revenue rather than efficiency. For example, if a drug is available in multiple vial sizes, using the optimal combination can reduce waste and lower costs. By requiring dose rounding policies and leveraging clinical pharmacist oversight, employers can avoid overuse and ensure cost-effective dosing strategies.

Quantity Limits
Implementing quantity limits on specialty medications prevents excess dispensing and waste. Specialty drugs are often high-cost, and without proper safeguards, patients may receive more medication than clinically necessary. By setting quantity limits based on FDA-approved indications and real-world utilization data, plan sponsors can minimize waste and prevent unnecessary costs.
Medical Drug Rebates
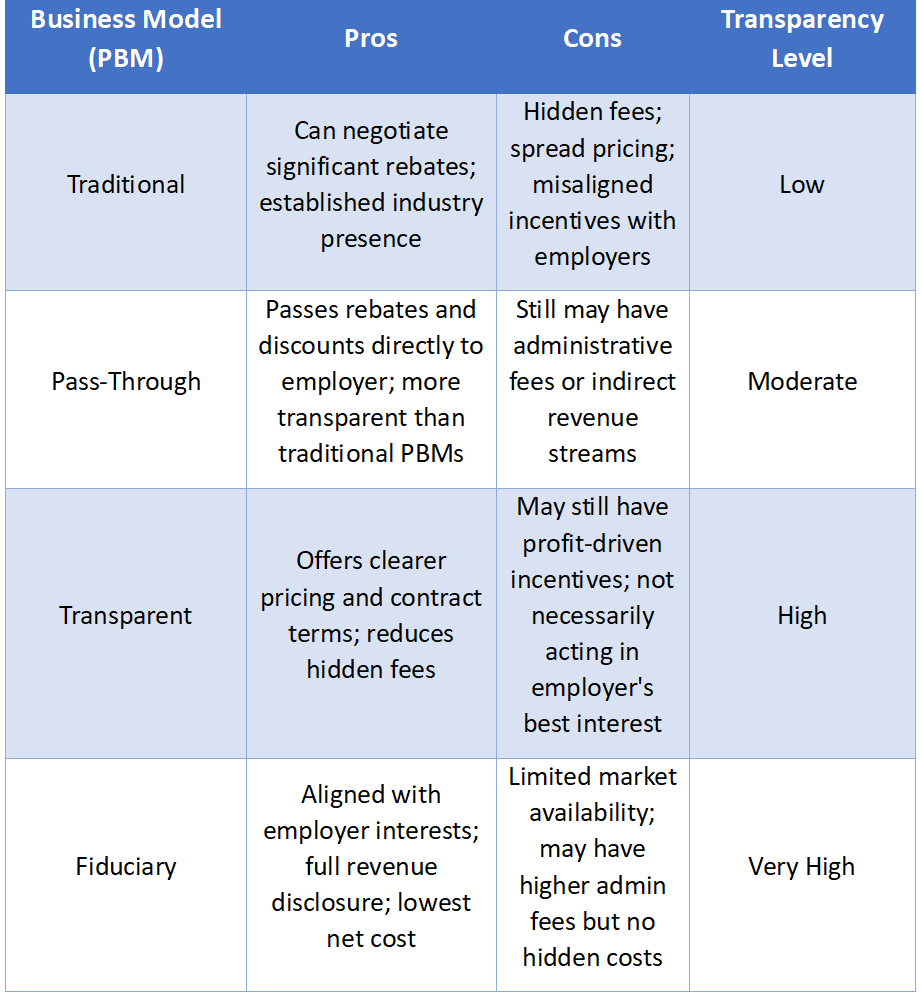
Rebates are a critical component of specialty drug reimbursement, yet they often remain opaque. Employers should demand full visibility into rebate agreements and ensure that all negotiated discounts are passed through. Fiduciary PBMs play a crucial role in securing transparent rebate structures that lower medical benefit drug costs while maintaining patient access to essential therapies.
Medical Formulary Management
A well-structured medical formulary helps steer utilization toward the most cost-effective therapies. By excluding high-cost drugs with limited clinical value and promoting biosimilars or lower-cost alternatives, formulary management can significantly reduce specialty drug spending. Employers should work with PBMs that take a fiduciary approach to formulary design, ensuring that decisions are based on clinical and financial value rather than hidden incentives.
Site of Care Management
Where a specialty drug is administered can dramatically impact cost. Hospital outpatient settings often charge significantly more for the same infusion therapy compared to in-home or alternate site infusion centers. Implementing a site-of-care program that redirects patients to lower-cost, clinically appropriate settings can yield substantial savings. Employers should leverage data analytics to identify opportunities for site-of-care shifts and implement incentives for members to choose lower-cost locations.
Conclusion
Medical benefit drug costs will continue to rise, but self-funded employers and plan sponsors have significant opportunities to manage these expenses more effectively. By focusing on clinical effectiveness, pricing validation, dose optimization, quantity limits, rebates, formulary management, and site-of-care strategies, organizations can take control of specialty drug spending without sacrificing patient outcomes. Those who fail to adopt a proactive reimbursement strategy risk excessive costs and financial inefficiencies. Employers must demand transparency, accountability, and a fiduciary approach from their PBM partners to drive sustainable savings in medical specialty reimbursement.