Court Rules in Favor of Cigna Over Anthem in $14.8B PBM Drug Overcharge Claim [Weekly Roundup]
PBM drug overcharge claim plus other news and notes from around the interweb:
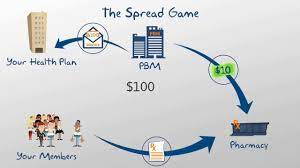
- Court Rules in Favor of Cigna Over Anthem in $14.8B PBM Drug Overcharge Claim. Cigna Corp. won a key part of a six-year legal dispute in which Anthem Inc. claimed it was overcharged for pharmacy benefits services, fending off the rival health insurer’s bid for $14.8 billion in damages. Anthem isn’t entitled to the billions it claimed were owed over prescription drug prices charged by Cigna’s Express Scripts unit, a federal judge in New York ruled Thursday. The court ruled that the contract didn’t require Express Scripts to guarantee competitive prices based on benchmarks, but only that it had to negotiate in good faith.
- Key Differences Between Fiduciary and Traditional Pharmacy Benefit Managers. Pharmacy Benefit Managers (PBM) are authorized to manage the benefit on their own behalf, with a wide range of restrictions and constraints that serve the PBMs interest, often at the client’s expense. On the other hand, a Fiduciary PBM manages the benefit without that conflict of interest, and with better transparency – looking out for the best interest of the client and plan participants only. What are the Key Differences Between Fiduciary and Traditional PBM Business Models?
- AHIP study claims hospitals charge double for specialty drugs compared to pharmacies. Hospitals on average charge double the price for the same drugs compared to those offered by specialty pharmacies, according to a new insurer-funded study released as federal regulators ponder a probe into the pharmacy benefit management industry. The study (PDF), released Wednesday by insurance lobbying group AHIP, comes as specialty pharmacies have grown in use among PBMs and payers to dispense specialty products. The study was released a day before a scheduled meeting Thursday of the Federal Trade Commission on whether to probe the competitive impact of PBM contracts and how they could disadvantage independent and specialty pharmacies.
- Preparing manufacturers for a changing copay landscape. The traditional pharmacy copay model, which was more commoditized by focusing on the value of each transaction and managing patient eligibility, is quickly shifting toward a patient focused format. What was a comfortable and familiar landscape to manufacturers has been challenged by accumulator and maximizer programs, and manufacturers are challenged to pivot to patient value-based plans, risk sharing models and other forward-looking strategies.
- Louisiana AG sues UnitedHealth, alleging drug overcharges in Medicaid. Louisiana Attorney General Jeff Landry has sued UnitedHealth Group, claiming that the healthcare and insurance giant has inflated drug charges in the state’s Medicaid program by billions. The suit was filed April 13 in state court, Bloomberg reported, and alleges that the company’s pharmacy benefit manager Optum Rx took advantage of the secrecy of the pharmacy supply chain to “needlessly” charge Medicaid billions for prescription drug benefits.