Early Pharmacy Claims Data from Exchange Enrollees Indicate High Usage
Now that exchanges are up and running, preliminary drug claims data is showing such a trend. The April 17 issue of Atlantic Information Services, Inc.’s Inside Health Insurance Exchanges (HEX) walks readers through data from two pharmacy benefit managers (PBMs) and what it means for insurers.
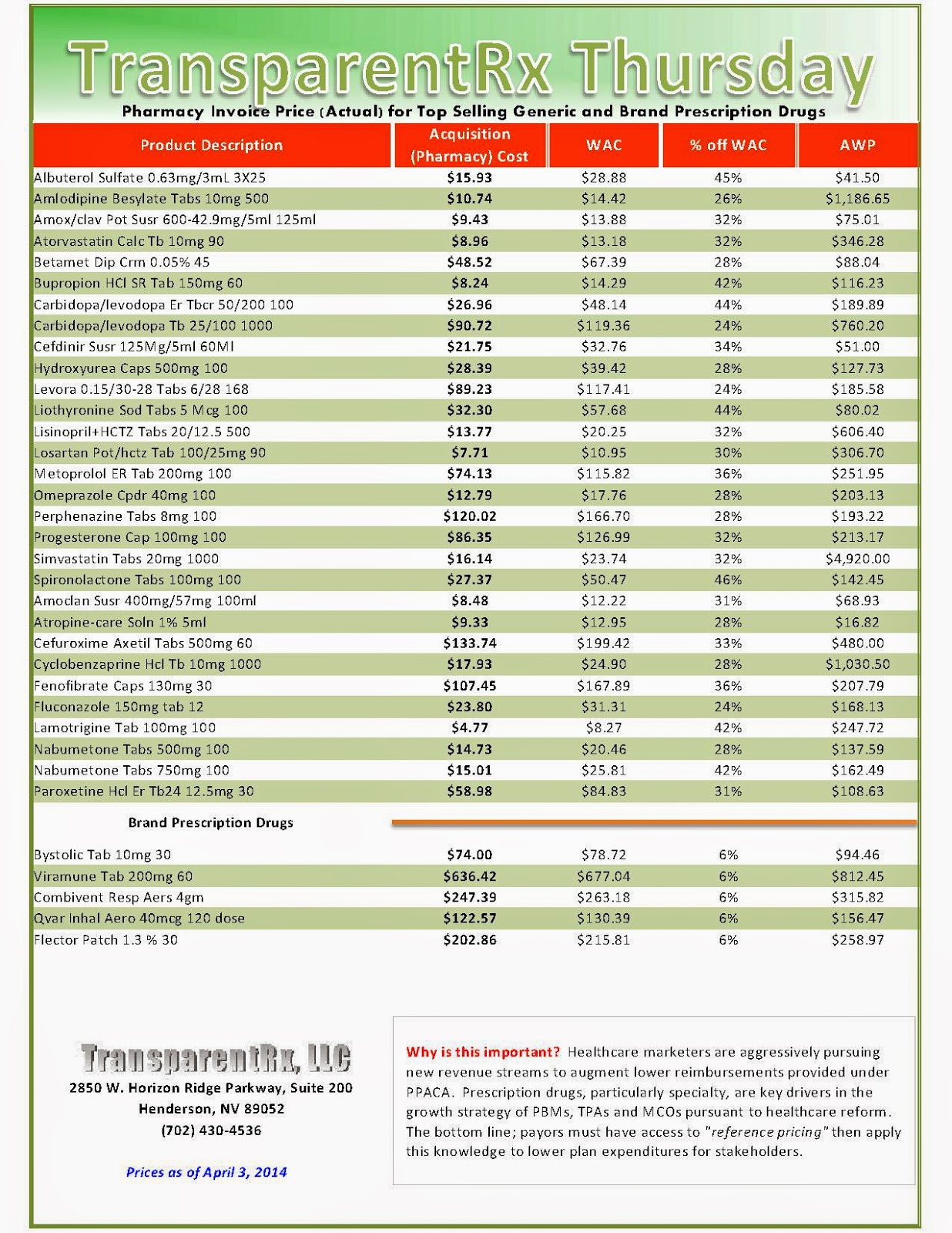
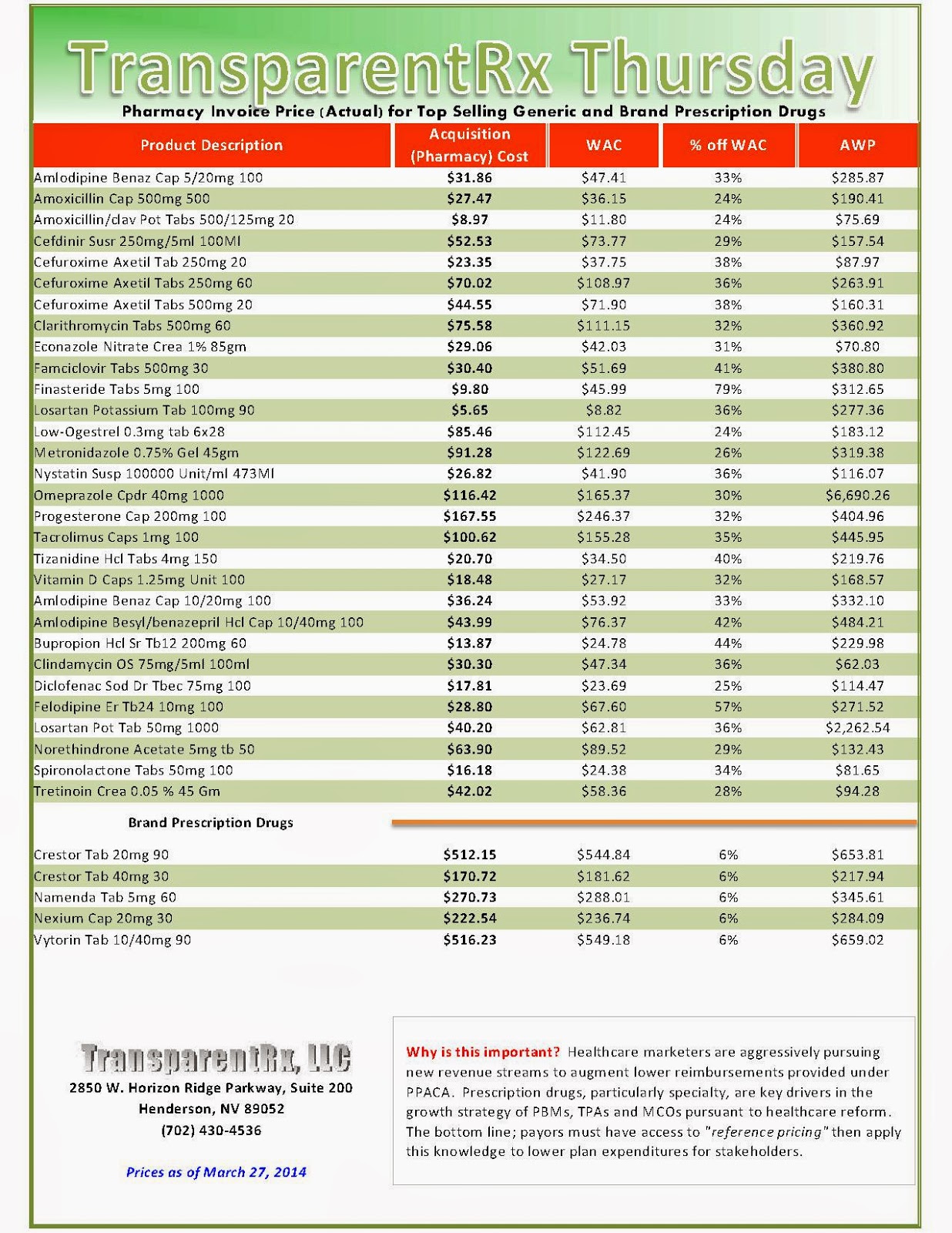
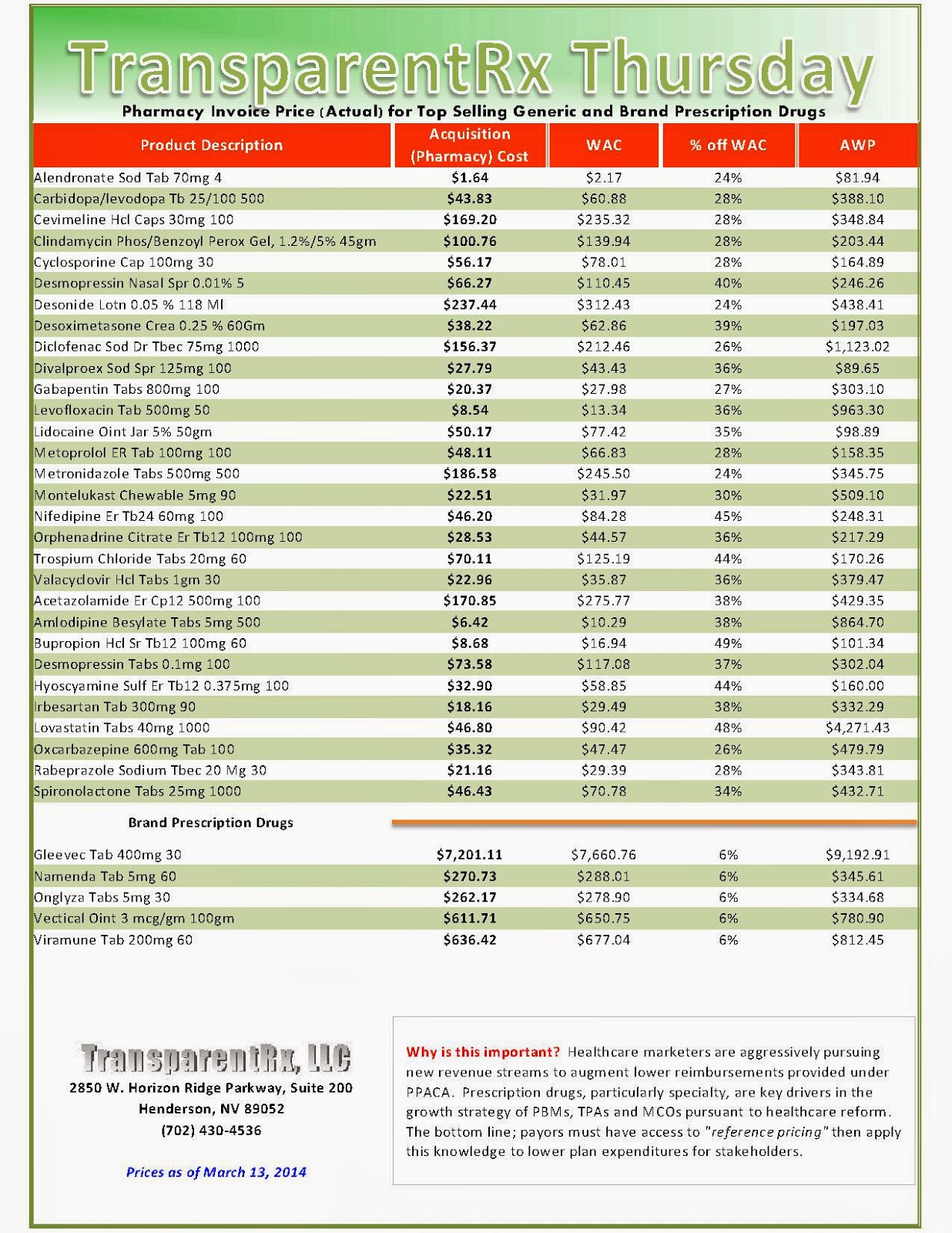
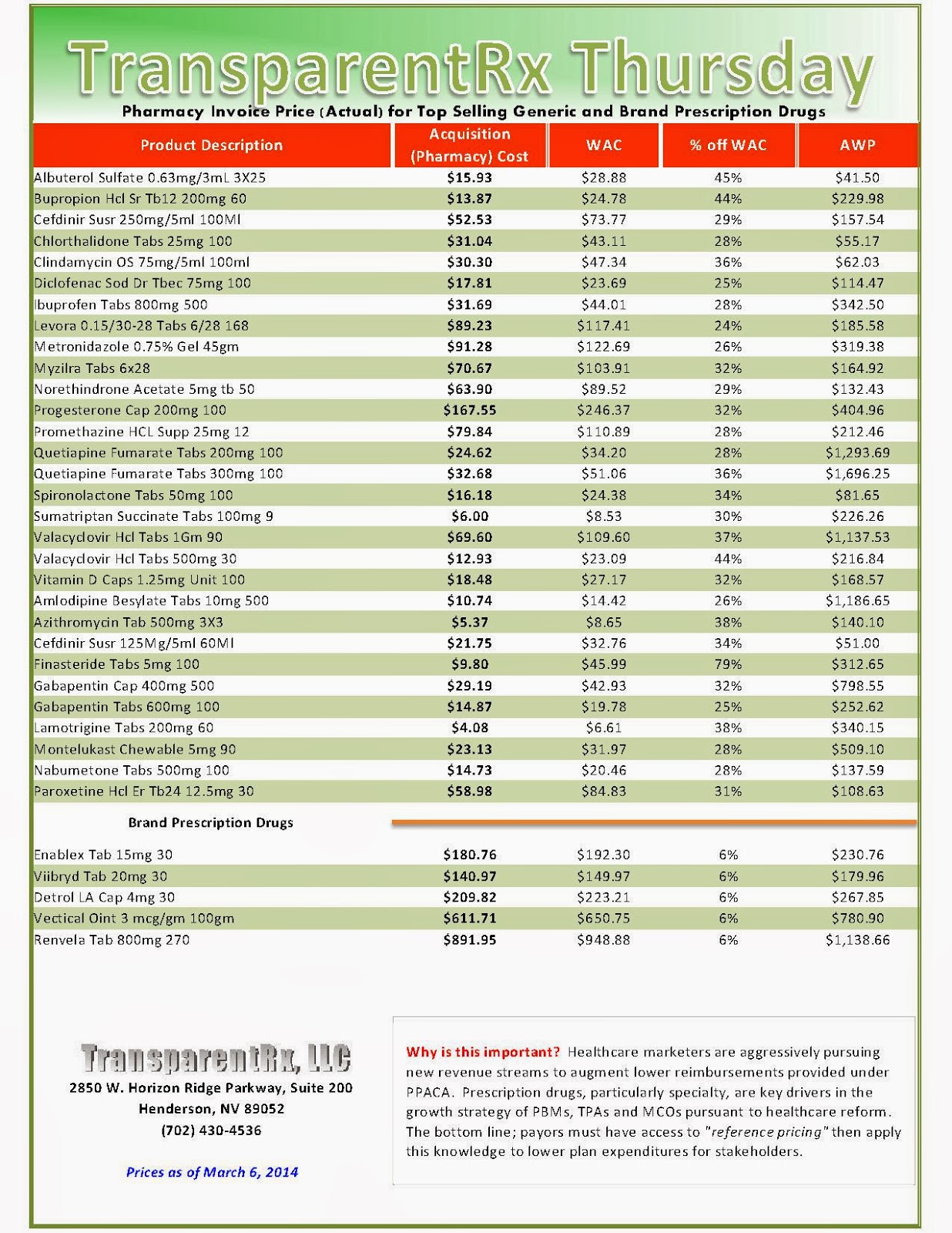
During the first two months of 2014, exchange enrollees were more likely to use costly specialty drugs when compared to those with coverage outside of the exchanges, according to preliminary claims data released April 9 by Express Scripts.
According to the early data, six of the 10 costliest medications used by exchange enrollees were specialty drugs versus four of the top 10 used by commercial health plan enrollees. Of total prescriptions filled for exchange plans, 1.1% was for specialty drugs, compared with 0.75% in commercial plans — a near-50% difference.
Read more: http://www.digitaljournal.com/pr/1867253#ixzz2zipbRF40

_1.jpg)

_1.jpg)

_1.jpg)

_1.jpg)