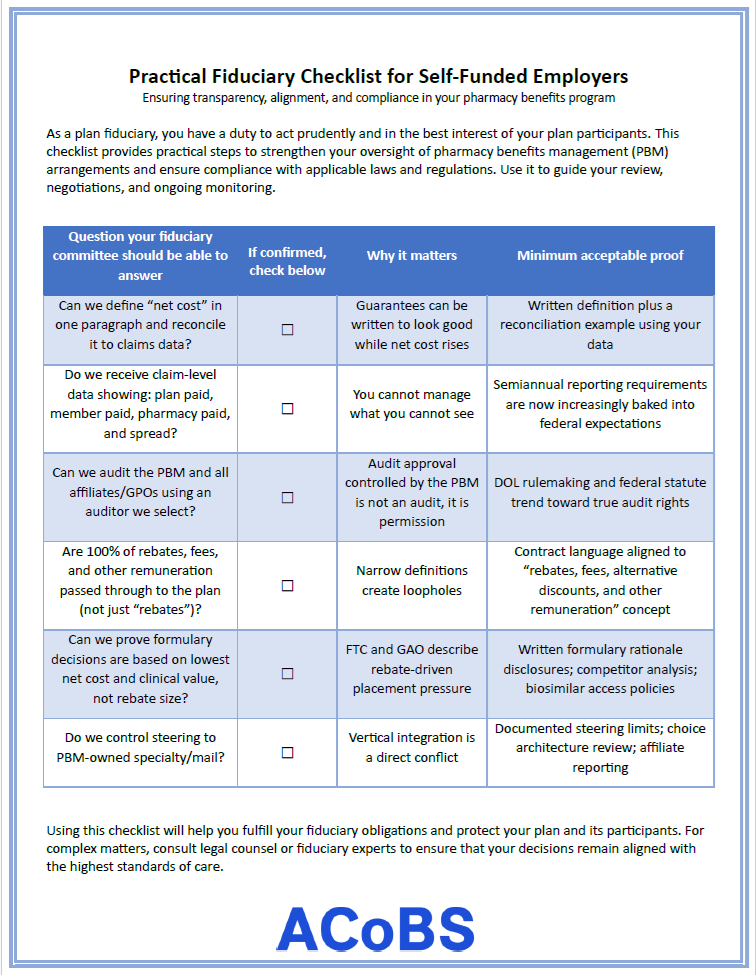
Self-funded employers operate under a prudent expert standard. The Consolidated Appropriations Act raised the bar. A good faith effort is not enough. Plan fiduciaries must understand what they are buying, what they are paying, and whether the arrangement serves participants, not intermediaries. A practical fiduciary checklist is not theoretical. It is operational.
- Confirm true independence. Require written disclosure of all direct and indirect compensation paid to your PBM and your consultant. Indirect revenue, side agreements, rebate aggregators, and affiliated entities matter. If your advisor receives compensation from a PBM, you do not have a buyer’s agent. You have a seller’s agent. Replace conflicted vendors if necessary.
- Define value before you define rebates. Rebates are not value. Net cost by drug class, appropriateness, waste reduction, and total cost of care are value. Demand reporting that shows ingredient cost, dispensing fee, member cost share, and all manufacturer revenue tied to your utilization. If you cannot see the full economics at the claim level, you cannot meet a fiduciary standard.
- Control the formulary. Your PBM’s P&T committee is not automatically aligned with you. Vertical integration and rebate-driven placement can bias decisions toward high-list-price drugs. Require a value-based formulary that prefers generics and biosimilars when clinically appropriate. Prohibit favoring a higher list price drug solely because it generates a larger rebate. Demand quarterly formulary updates and written justification for material changes.
- Tighten utilization management. Prior authorization approval rates north of 90 percent signal process failure. Protocols should be clinically grounded, documented, and consistently applied. Prohibit off-label expansion designed to increase rebate flow. Insist on reporting that shows approval rates, step therapy compliance, and exception patterns by drug class. Own the data. You must have full access to claims files, historical data, and rebate invoices. Require clear identifiers for 340B claims, specialty drugs, MAC pricing, coupon usage, and exclusions from guarantees. If you cannot independently reprice claims, conduct market checks, and audit rebate agreements, you are relying on representations, not evidence.
- Eliminate guarantee games. Forbid offsets where overperformance in one guarantee masks underperformance in another. Define rebates broadly to include all manufacturer payments, not just what the PBM chooses to label as a rebate. Close loopholes tied to definitions of generic, specialty, or excluded drugs.
- Audit aggressively. Retain an independent auditor with unrestricted access to contracts, pharmacy records, and rebate agreements. No blackout periods. No PBM veto over auditor selection. Annual audits should assess pricing, rebate pass-through, formulary compliance, and contract adherence.
- Separate 340B economics. Require separate identification and pricing treatment of 340B claims. Do not allow inflated list pricing to persist without rebate offset. If 340B savings are not passed through, you are subsidizing intermediaries.
Fiduciary governance in pharmacy benefits is not about squeezing another basis point from a discount off AWP. It is about knowledge. Knowledge of definitions. Knowledge of financial flows. Knowledge of clinical appropriateness.
If you do not understand the mechanics, you cannot discharge the duty. If you do understand them, you can realign the system to serve the only constituency that matters: your plan participants.
How to Know If You Are Falling Short
This checklist is a governance test. Missing one item may signal a process gap. Missing two or three signals exposure. If the gaps are administrative, such as delayed reporting or incomplete benchmarking, you likely have an operational weakness that can be corrected.
If the gaps involve financial transparency, audit rights, data ownership, conflicted compensation, or formulary control, the risk is structural. These are not minor deficiencies. They directly affect whether plan assets are being managed solely in the interest of participants, as required under a prudent expert standard.
You should assume you are out of alignment if:
- You cannot document every source of PBM and consultant compensation tied to your plan.
- You do not have full audit rights, including access to rebate agreements and subcontractors.
- You cannot independently reprice claims or validate net cost by drug class.
- You permit guarantee offsets that mask underperformance.
- You rely on your PBM’s formulary decisions without independent review.
Two or three misses in these areas are not cosmetic. They mean you cannot verify alignment. And if you cannot verify alignment, you cannot demonstrate prudent oversight. The practical rule is simple: If a gap limits transparency or independence, treat it as a fiduciary risk until corrected. Gaps become failures only when they are ignored.
How We Can Work Together
Whether you’re a plan sponsor trying to get control of pharmacy spend, or a broker guiding clients through PBM decisions, education is the fastest way to improve outcomes. If you want a focused, high-value session your team can actually use, here are several ways we can work together.
Option 1: Get Certified
American College of Benefit Specialists (ACoBS) equips benefits professionals with practical knowledge across pharmacy, medical, retirement, and voluntary benefits. Organizations working with ACoBS-certified consultants gain better plan oversight, stronger vendor accountability, and more disciplined cost control. The certification signals a clear commitment to fiduciary guidance and protecting plan assets.
Option 2: Book a Webinar
A clean, educational session for employers, brokers, or TPAs. We’ll cover the most common PBM profit tactics, how to spot contract red flags, and what a fiduciary standard of care looks like in pharmacy benefits. Great for client education and thought leadership.
Option 3: Join the Virtual Roundtable
Bring your internal team (HR, Finance, and Benefits) or your broker group. I’ll lead a live discussion focused on PBM oversight, cost drivers, and what to ask your PBM right now. You’ll leave with a short action list you can use immediately.
Option 4: Get a Quote
Pharmacy benefits now rival medical spend for many plans. Yet most are still governed by contracts few have fully read and pricing models few can clearly explain. That is a fiduciary risk, not just a cost issue.
If you want lower spend, tighter oversight, and alignment you can defend in front of a board or audit committee, act with intent. Certify your team. Educate your clients. Pressure test your PBM. Run an RFP that exposes the full economics.
Hope is not a strategy. Oversight is. The employers who win in pharmacy benefits are not lucky. They are informed, disciplined, and unwilling to outsource accountability.