Pharmacy benefits managers have evolved from claims processing to home delivery, managing formulary, specialty pharmacy, and negotiating with manufacturers.
With the ongoing backlash against them—complaints of lack of transparency and regulation, conflicts of interest created through owning specialty and mail order pharmacies, perverse incentives, and rising pharmacy costs—PBMs may decide to make some changes in how they operate.
 |
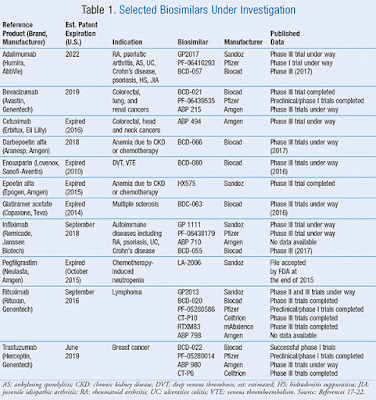
| Table 1 |
Susan Pilch, JD, Vice President, Policy and Regulatory Affairs for the National Community Pharmacists Association (NCPA), believes that heightened demand from employers for information about where their pharmacy dollars are going and what their contracts mean could force PBMs to come to the table and address these concerns.
But can the industry live without PBMs, she wondered. “We will always need claims processors—a valid PBM activity—but we would like to move PBMs away from their role as gatekeeper of drugs and their costs,” she said. “We need oversight to hold PBMs accountable, but it’s hard to place demands when you don’t know what PBMs are doing.”
Tyrone’s comment: A fiduciary-model PBM addresses these concerns yet spokespersons at the highest levels of organizations like NCPA aren’t sufficiently talking about it. Have they written the fiduciary model off as unattainable because behemoth PBMs say they won’t provide it? Big breakthroughs occur with persistence despite those who say it isn’t possible.
Mark Merritt, President and CEO of the Pharmaceutical Care Management Association (PCMA), predicts that PBMs will assume a more clinical focus as drugs continue to be more complex. “PBMs have been at the forefront of utilization data and, as genomics leads to more personalized medicine, we can provide claims data,” he said.
He also foresees greater collaboration with health plans as more specialty drugs enter the marketplace and with physicians who require access to data about formularies—what specifically is on them and how many are generics versus brands.
In defense of what many stakeholders call a lack of transparency on the part of PBMs, Merritt noted that as plan sponsors become more sophisticated about benefits by consulting experts, more transparency will evolve. However, he believes that transparency has always existed, but that purchasers have failed to fully take advantage of it.
Tyrone’s comment: Did you catch that? Mark is essentially repeating what I’ve been writing about for the past seven years. Radical transparency, from PBMs, is attainable provided plan sponsors are willing to invest the time and money required to become more sophisticated and attentive purchasers.
David Lansky, PhD, President and CEO of the Pacific Business Group on Health (PBGH), questions whether PBMs will be able to prove that their performance, transparency, and effectiveness work well enough to justify their role or whether other services and structures will emerge. On the other hand, he said that PBM functions are valuable and that his members want these services at the lowest cost to provide the right medications with the least hassle.
“Ultimately, the responsibility of total cost of care should be in the hands of a care system. If they are going to manage a population, they need to manage all the necessary resources for achieving the best outcomes at a reasonable, competitive cost,” Lansky says.
“With drugs now accounting for close to 25% of total spending, it’s essential that the care system have the tools and responsibility to manage medication spending, as well as other medical services,” he continues.
“Employers need a business partner with pharmacy expertise who understands opportunities and oversees the business,” he says. “It’s a clinically complex area. No employer wants to be in the middle of deciding whether an employee should receive a certain drug.”
[Source]