Three Underappreciated Reasons for Micromanaging Pharmacy Benefits
My pharmacy background started with Eli Lilly & Company, a top twenty pharmaceutical manufacturer by sales. It was one of the best jobs I ever had and not just because of the perks. We talked a lot about helping patients get better which made me feel good about what I was doing. That being said, I’m not naive. We wanted to sell as much type 2 diabetes products as we could. To do that, we relied heavily on lax formulary and drug utilization management on the part of plan sponsors. Here are three underappreciated reasons for micromanaging pharmacy benefits.
Reason #1 – Drugmakers are making it easier to get access to high-cost specialty drugs
Prescription medicine is moving increasingly online with direct-to-consumer advertising by adopting a more assertive catchphrase: Talk to a doctor now. I haven’t checked every brand drug, but I suspect all of them have a dedicated website. These websites are now incorporating built-in buttons Talk to a Doctor Now for everything from sickle cell disease to migraine drug therapies. One communication about IBS or irritable bowel syndrome even reads, “you deserve to feel better.”
Reason #2 – PBMs too often permit high-cost brand drugs to be dispensed in place of lower cost generic equivalents
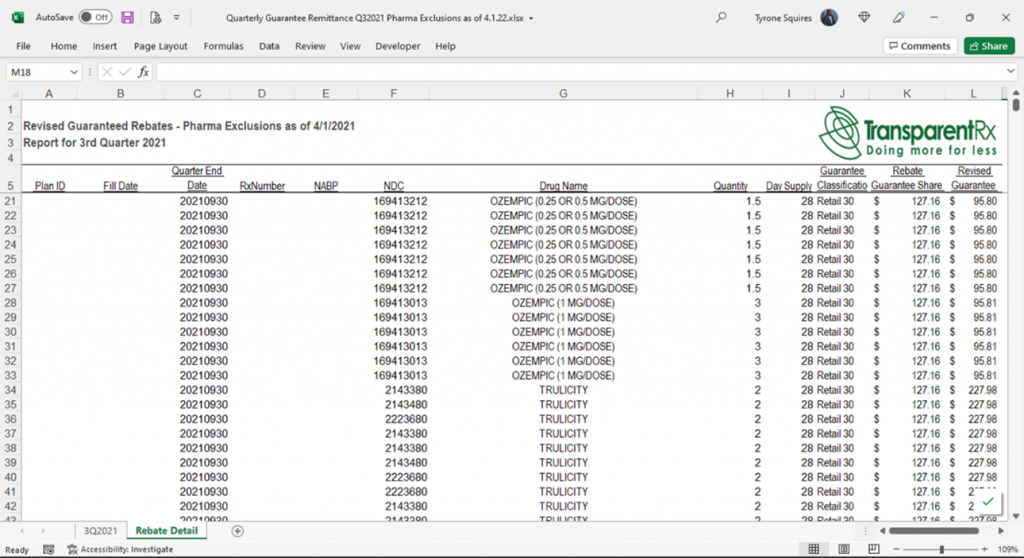
When plan sponsors forgo efficiency for participant satisfaction PBMs take financial advantage of the decision. High participant satisfaction usually means the patient getting the exact prescription drug, prescribed by the doctor, without any scrutiny. In my time with Eli Lilly, I took a territory ranked #600 to #11 in one year by persuading doctors to dispense a new type 2 diabetes brand drug (Actos) over a proven and much less costly generic Metformin. Actos provided no significant A1C improvements compared to metformin. A1C is the primary performance metric for antidiabetic agents. It is a simple blood test that measures average blood sugar levels. Below is an audio file (click the image) of a similar conversation between a PBM and broker. The president of a brokerage firm based in the south sent this to me. The PBM has forced Zytiga over its lower cost generic equivalent Abiraterone Acetate. My instincts tell me this PBM has a distribution deal for Zytiga. Depending upon the pharmacy, the retail price of brand Zytiga is easily 30x the generic version.
Reason #3 – One of the largest electronic prior authorization (ePA) companies in the world, CoverMyMeds, is owned by a drug wholesaler. Do I need to say more?
Three Underappreciated Reasons for Micromanaging Pharmacy Benefits Conclusion
Employers have been reluctant actors in the U.S. pharmacy distribution and reimbursement system, relying on third parties who may not have their best interests in mind. Some companies, like Honeywell and Caterpillar, have taken tough steps to control costs, with no loss in employee satisfaction. It is impossible to run an efficient pharmacy benefits management program without elements of micromanagement. Micromanagement in pharmacy benefits means every claim gets scrutinized with a focus on the lowest net cost. To minimize the impact of PBM, pharmaceutical manufacturer, and drug wholesaler efforts to pad their own pockets at employers’ expense, employ and measure the effectiveness of drug utilization management tools like step therapy, prior authorization, and mandatory generic enforcement programs. Oh, and don’t forget about DAW codes.




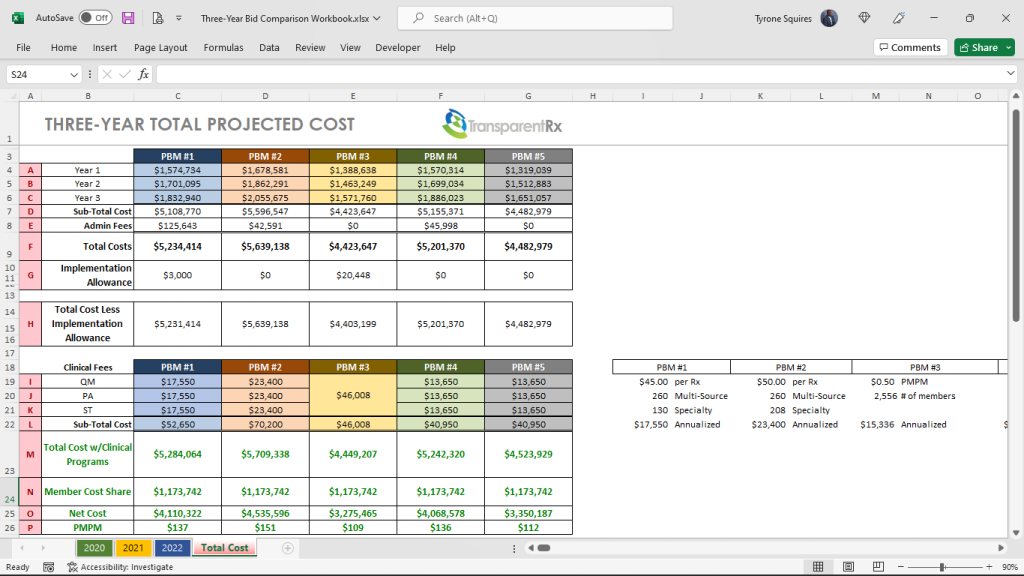
 Once all bids are collected the consultant then plugs them into their in-house Excel spreadsheet or a third-party bid analyzer software platform. This is where the problems begin more on that in a bit.
Once all bids are collected the consultant then plugs them into their in-house Excel spreadsheet or a third-party bid analyzer software platform. This is where the problems begin more on that in a bit.