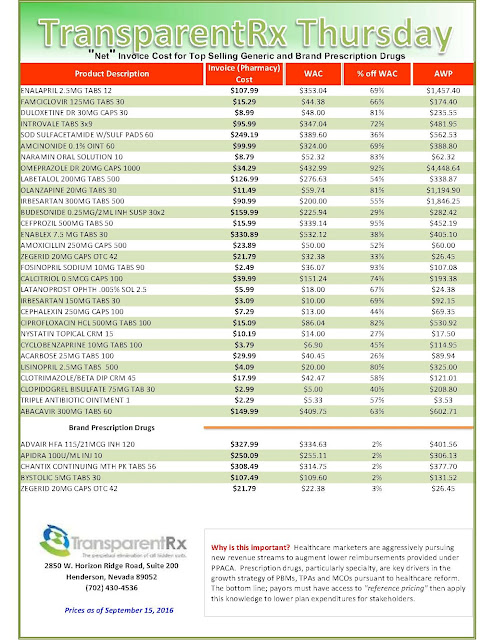
“Gross” Invoice Cost for Top Selling Generic and Brand Prescription Drugs – Volume 135
The costs shared below are what the pharmacy actually pays; not AWP, MAC or WAC. The bottom line; payers must have access to “reference pricing.” Apply this knowledge to hold PBMs accountable and lower plan expenditures for stakeholders.
How to Determine if Your Company [or Client] is Overpaying
Step #1: Obtain a price list for generic prescription drugs from your broker, TPA, ASO or PBM every month.
Step #2: In addition, request an electronic copy of all your prescription transactions (claims) for the billing cycle which coincides with the date of your price list.
Step #3: Compare approximately 10 to 20 prescription claims against the price list to confirm contract agreement. It’s impractical to verify all claims, but 10 is a sample size large enough to extract some good assumptions.
Step #4: Now take it one step further. Check what your organization has paid, for prescription drugs, against our pharmacy cost then determine if a problem exists. When there is a 5% or more price differential (paid versus actual cost) we consider this a problem.
Multiple price differential discoveries means that your organization or client is likely overpaying. REPEAT these steps once per month.
— Tip —
Always include a semi-annual market check in your PBM contract language. Market checks provide each payer the ability, during the contract, to determine if better pricing is available in the marketplace compared to what the client is currently receiving.
When better pricing is discovered the contract language should stipulate the client be indemnified. Do not allow the PBM to limit the market check language to a similar size client, benefit design and/or drug utilization. In this case, the market check language is effectually meaningless.
Note: Prices listed herein are gross thus do not account for rebates, discounts or other purchase incentives which ultimately reduces the net cost.
Chicken Soup for the Self-Funded Employer: Foolproof PBM Contracts
 Having spent all of my post-graduate years (15) in the pharmaceutical industry, I’ve come to know two immutable pharmacy benefit management principles and they are:
Having spent all of my post-graduate years (15) in the pharmaceutical industry, I’ve come to know two immutable pharmacy benefit management principles and they are:1) You get what you exactly measure [payer-side]
2) The things that you measure, costs and outcomes, will get gamed
Analytics may help ease the pain but don’t alone solve the problem which is excessive overpayments. Furthermore, analytics can worsen the problem because purchasers rely too heavily on it. In other words, don’t rely solely on analytic software programs and all the neat reports they spit out especially if what’s being measured is inherently flawed (i.e. AWP and MAC).
Eliminating overpayments is done two ways:
➤ Sophisticated purchasers, of PBM services, with super strong negotiating skills lead the procurement of services.
 |
| [Click to Enlarge] |
Douglas Adams wrote in Mostly Harmless, “a common mistake that people make when trying to design something completely foolproof is to underestimate the ingenuity of complete fools.” I’m reminded of this each time I read something about the Anthem, Express Scripts dispute or Wells Fargo.
One slide from my “don’t miss” webinar Tuesday September 13 at 3:00 PM ET
This slide is a sledge hammer on the status quo and it will enable you to create a compelling case for change. It’s also the exact message non-fiduciary PBMs don’t want you to hear. Want to know more?
Register: https://attendee.gototraining.com/rt/3034343502849349634
A snapshot of what you will learn in this 30 minute webinar:
- Hidden Cash flows in the PBM Industry
- The definition of binding transparency (hint: there is no standard industry definition for transparency)
- How to calculate cost of pharmacy benefit manager services or CPBMS
- Why Anthem, Inc. sued Express Scripts Holding Co.
- The difference between actual acquisition cost and MAC
See you Tuesday September 13 at 3:00 PM ET!
Sincerely,
Tyrone D. Squires, MBA
TransparentRx
2850 W Horizon Ridge Pkwy., Suite 200
Henderson, NV 89052
866-499-1940 Ext. 201
P.S. Yes, it’s recorded. I know you’re busy … so register now and we’ll send you the link to the session recording as soon as it’s ready.
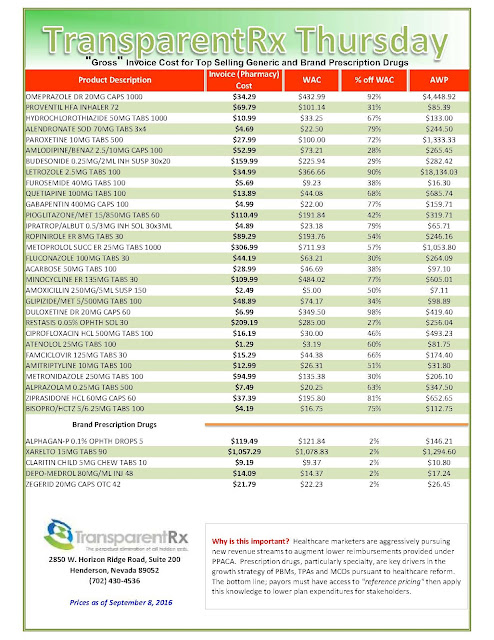
“Gross” Invoice Cost for Top Selling Generic and Brand Prescription Drugs – Volume 134
The costs shared below are what the pharmacy actually pays; not AWP, MAC or WAC. The bottom line; payers must have access to “reference pricing.” Apply this knowledge to hold PBMs accountable and lower plan expenditures for stakeholders.
Step #1: Obtain a price list for generic prescription drugs from your broker, TPA, ASO or PBM every month.
Step #2: In addition, request an electronic copy of all your prescription transactions (claims) for the billing cycle which coincides with the date of your price list.
Step #3: Compare approximately 10 to 20 prescription claims against the price list to confirm contract agreement. It’s impractical to verify all claims, but 10 is a sample size large enough to extract some good assumptions.
Step #4: Now take it one step further. Check what your organization has paid, for prescription drugs, against our pharmacy cost then determine if a problem exists. When there is a 5% or more price differential (paid versus actual cost) we consider this a problem.
Multiple price differential discoveries means that your organization or client is likely overpaying. REPEAT these steps once per month.
— Tip —
Always include a semi-annual market check in your PBM contract language. Market checks provide each payer the ability, during the contract, to determine if better pricing is available in the marketplace compared to what the client is currently receiving.
When better pricing is discovered the contract language should stipulate the client be indemnified. Do not allow the PBM to limit the market check language to a similar size client, benefit design and/or drug utilization. In this case, the market check language is effectually meaningless.
Note: Prices listed herein are gross thus do not account for rebates, discounts or other purchase incentives which ultimately reduces the net cost.
[Podcast] Rx Drugs and the U.S. Health System – A Conversation About Drug Prices
It’s nice to be able to fill in some of the holes when dealing with a complicated issue. So, I strongly recommend you read these two blog posts before listening to the podcast.
1) How Pfizer set the cost of its new drug at $9,850 a month
2) Express Scripts generates top-line revenue of $76.63 per claim!
My big takeaway is that Express Scripts is extremely arrogant; lecturing manufacturers on how to run their businesses. Imagine for a second the strong arm tactics ESI might use when negotiating rebates not for the sole benefit of plan sponsors but its own pockets. Click play to listen…
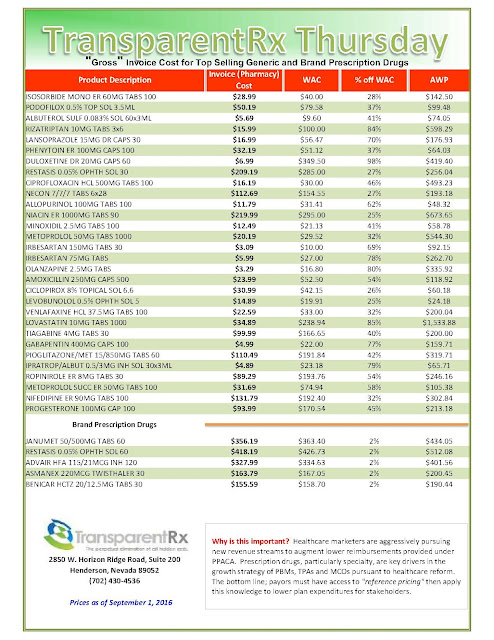
“Gross” Invoice Cost for Top Selling Generic and Brand Prescription Drugs – Volume 133
The costs shared below are what the pharmacy actually pays; not AWP, MAC or WAC. The bottom line; payers must have access to “reference pricing.” Apply this knowledge to hold PBMs accountable and lower plan expenditures for stakeholders.
Step #1: Obtain a price list for generic prescription drugs from your broker, TPA, ASO or PBM every month.
Step #2: In addition, request an electronic copy of all your prescription transactions (claims) for the billing cycle which coincides with the date of your price list.
Step #3: Compare approximately 10 to 20 prescription claims against the price list to confirm contract agreement. It’s impractical to verify all claims, but 10 is a sample size large enough to extract some good assumptions.
Step #4: Now take it one step further. Check what your organization has paid, for prescription drugs, against our pharmacy cost then determine if a problem exists. When there is a 5% or more price differential (paid versus actual cost) we consider this a problem.
Multiple price differential discoveries means that your organization or client is likely overpaying. REPEAT these steps once per month.
— Tip —
Always include a semi-annual market check in your PBM contract language. Market checks provide each payer the ability, during the contract, to determine if better pricing is available in the marketplace compared to what the client is currently receiving.
When better pricing is discovered the contract language should stipulate the client be indemnified. Do not allow the PBM to limit the market check language to a similar size client, benefit design and/or drug utilization. In this case, the market check language is effectually meaningless.
Note: Prices listed herein are gross thus do not account for rebates, discounts or other purchase incentives which ultimately reduces the net cost.
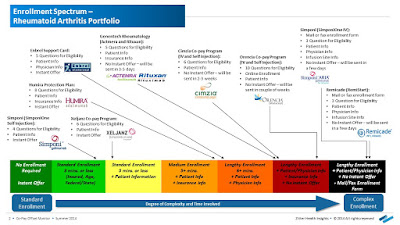
The co-pay card debate simmers, as payers push back
Devised to shoulder some of the cost burden of prescription drugs, manufacturer co-pay card programs have been tied to improved adherence rates and reduced barriers to the discounted medications. At the same time, payers — insurers and PBMs alike — are crying foul.
While some industry veterans sing the praises of co-pay assistance programs, others are eager for a more evenhanded and efficient solution that will achieve the same degree of cost savings. In fact, the co-pay card appears to be stirring the controversy pot more than ever. Indeed, the question seems to have become: What will make it boil over?
UNHAPPY PAYERS
 |
| Click to Enlarge |
But after more than a decade as an industry staple, the instant-rebate tactic has come under fire. Andrew Miller, VP of operations at pharmacy benefits manager MeridianRx, has grown increasingly concerned with the damaging effects of co-pay cards on payers. Consider insured patients who have been prescribed AbbVie’s Humira for their rheumatoid arthritis at $4,000 per month. After insurance and co-insurance kick in, they’re on the hook for $1,000 a month. But wait — the manufacturer just happens to have a co-pay coupon, which reduces the cost to zero.
What’s the problem, you ask? The insurer and the PBM didn’t get the memo. After six months of taking and paying for the medication, the PBM’s records show the patient paying $6,000 and capping out his out-of-pocket maximum — when, in fact, the patient has paid nothing — the drug company picked up the tab. “There needs to be collaboration to flag that a co-pay coupon has been used,” Miller stresses.
————————-
Tyrone’s comment: In the interest of full disclosure I know Andrew personally so my comments will not come as a shock to him. My position is that co-pay cards are a good thing for patients and plan sponsors but not so much for non-fiduciary PBMs.
Here’s a quick story.
A few months back my mom shared with me that she was not on speaking terms with my uncle so I asked why. They often have these disagreements and all is back to normal in a few days. Apparently, she hired my uncle to repair her washer. Something had gone wrong such that it wouldn’t turn. It was an old top loading washer; my mom is frugal like that and won’t spend money on anything new unless it’s the last resort.
They had agreed on a price of $100 plus parts. Turns out my uncle looked at the back of the machine adjusted some sort of wire and the job was done in 30 seconds! My mom believed she overpaid and didn’t want to fork over the $100. She is wrong just like Andrew and here’s why.
1) The payer has agreed to its share of the cost so why be concerned with how the patient delivers their end of the bargain hence the washer story. Payers need to be more concerned about the manufacturer revenue PBMs are earning [and not passing back] than the assistance patients are receiving for drugs which don’t qualify for rebates in the first place. This leads me to bullet number two.
2) This is more about the rebate dollars PBMs aren’t getting. Manufacturers offer incentives (rebates, fees, discounts, expenses etc..) in exchange for market share (preferred formulary tier) and when they don’t get market share they don’t pay rebates or not nearly as much. So when a patient is prescribed a non-preferred medication it is likely in lieu of one that is preferred which means the PBM gets zero or less rebate dollars. Instead of paying the money (rebates) to PBMs, manufacturers are reallocating it to patients in the form of lower out-of-pocket costs to boost market share.
3) Insurers will say they are still paying the same high prices with co-pay cards. The truth is they aren’t paying the same high prices because the tier determines their cost share. Tier 1 might be 80% cost to the insurer while Tier 3 is 50%, for example. If a plan sponsor’s formulary isn’t at least four tiers that is the problem not the co-pay cards. It is true rebates reduce net plan costs. But, so too do lower cost shares.
4) The less money patients pay out-of-pocket the less likely they’re to be non-adherent which theoretically means reduced physician and hospital costs for the plan sponsor.
As a fiduciary PBM, I could care less if a manufacturer is willing to fork over $1000, on a patients behalf, for a product we didn’t prefer or left completely off the formulary. We manage our formularies for outcomes and cost-effectiveness not for profit. Any revenue we receive from a manufacturer is passed back 100% to the plan sponsor which ultimately reduces net plan costs.
When two parties enter into an agreement one shouldn’t get upset how the other lives up to their end of the bargain provided it is done ethically and legally. Plan sponsors who don’t like co-pay cards probably agree with my mother’s initial reaction and have been influenced, either directly or indirectly, by non-fiduciary PBMs. My mom eventually paid the $100 now her and my uncle are again on good terms at least for now.
————————-
THE ROCKY BACKGROUND
As prescription drug prices skyrocket, most notably for specialty medications, some consumers have simply been priced out of certain treatments. In theory, the co-pay card seems the perfect fix, lowering out-of-pocket expenses for commercially insured or cash-paying patients and, in doing so, expanding their treatment options.
“Adherence to doctor’s orders is one of the biggest challenges in the industry,” says Mike Boken, managing partner at BioCentric. And cost is arguably one of the biggest barriers to medication adherence. In fact, 27% of insured patients report a medication’s cost as the main reason for not filling a prescription, according to a Kaiser Family Foundation tracking poll.
It’s difficult to measure just how much cost affects a patient’s ability — or willingness — to follow through with a prescribed medication. According to Boken, cost may be a major influence, but it’s not the only driver affecting adherence rates. “Sometimes adverse events can affect the numbers. Sometimes a patient simply doesn’t like taking a medication,” he says.
Either way, medication cost is an issue for providers, too. Physicians often factor in the depth of a patient’s pockets when prescribing a new medication — and therefore they have been among the biggest and most vocal supporters of co-pay coverage programs. In a CMI/Compas study of promotional preferences, physicians surveyed across nine specialties placed a higher value on patient assistance programs than sample and voucher programs.
Millennial physicians, in particular, are hardwired to think about pricing and often pepper sales reps with questions about coverage and patient costs. “Younger docs grew up with these programs,” Boken says. “They’re still trained to use generics first, but they’re open to co-pay programs.”
But Boken stresses that cost is neither a singular nor an isolated driver. “Newer products usually have some points of differentiation from the generic older products, but the clinical benefit has to be there,” he adds. “Sometimes when we talk about co-pays and payer issues, we lose sight of that.”
Bob Hastings, VP of marketing at co-pay program provider TrialCard, counters that co-pay cards give physicians more flexibility in treatment options. “Physicians are trained to be the experts. We prefer they make a therapeutic choice on behalf of a patient rather than on the formulary’s wishes.”
Read more >>
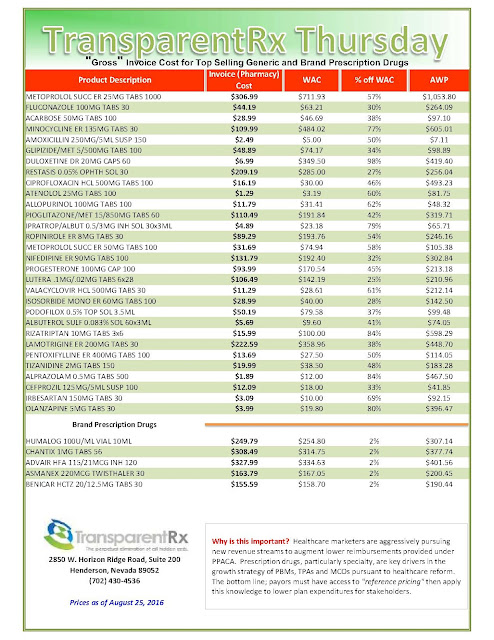
Reference Pricing: Actual Acquisition Cost (AAC) for Top Selling Generic and Brand Prescription Drugs – Volume 132
The costs shared below are what the pharmacy actually pays; not AWP, MAC or WAC. The bottom line; payers must have access to “reference pricing.” Apply this knowledge to hold PBMs accountable and lower plan expenditures for stakeholders.
Step #1: Obtain a price list for generic prescription drugs from your broker, TPA, ASO or PBM every month.
Step #2: In addition, request an electronic copy of all your prescription transactions (claims) for the billing cycle which coincides with the date of your price list.
Step #3: Compare approximately 10 to 20 prescription claims against the price list to confirm contract agreement. It’s impractical to verify all claims, but 10 is a sample size large enough to extract some good assumptions.
Step #4: Now take it one step further. Check what your organization has paid, for prescription drugs, against our pharmacy cost then determine if a problem exists. When there is a 5% or more price differential (paid versus actual cost) we consider this a problem.
Multiple price differential discoveries means that your organization or client is likely overpaying. REPEAT these steps once per month.
— Tip —
Always include a semi-annual market check in your PBM contract language. Market checks provide each payer the ability, during the contract, to determine if better pricing is available in the marketplace compared to what the client is currently receiving.
When better pricing is discovered the contract language should stipulate the client be indemnified. Do not allow the PBM to limit the market check language to a similar size client, benefit design and/or drug utilization. In this case, the market check language is effectually meaningless.
Note: Prices listed herein are gross thus do not account for rebates, discounts or other purchase incentives which ultimately reduces the net cost.
Hand caught in cookie jar, United Healthcare changing drug overpayment program
If you’ve held a 15-minute introductory phone conversation with me then you’re aware of the hidden cash flow tactic referred to as clawbacks.
Our “Medical Waste” investigative series showed how United, the nation’s largest health insurer, and Optum, its pharmacy benefit manager, overcharged some customers for prescription medication. The practice forced many customers to pay a copay that’s higher than the cost of the drug. United then claws back the extra money from the pharmacist. Optum labeled it an “overpayment program.”
“The hand in the cookie jar has been caught,” says Doug Hoey of the National Community Pharmacists Association. “There’s an old saying that sunlight is the best disinfectant. And I think some sunlight has been poured into their situation, and they’re trying to make the best of it. “
United sent us this statement:
“We have reviewed our pharmacy benefits and will update our plans to ensure UnitedHealthcare members pay the lowest price at the pharmacy.”
When we asked if this meant United plans to eliminate the “overpayment program” that forced customers to unknowingly overpay for prescriptions, United responded:
“Once fully insured customers move to the updated benefit plans, our members will pay the lowest price at the pharmacy and the repayment program will no longer be necessary.”
Tyrone’s comment: Wait, what about self-funded employers? Self-funded employers should be checking to verify these overpayments aren’t occurring within their plans. Higher OOP (out-of-pocket) expenses for patients leads to non-adherence which ultimately means increased hospital or physician costs.
“They would never say that they are doing something they shouldn’t be doing,” Hoey says. “But the fact that they’re changing their practices… to me, that’s an admission that they were over the line.”
We kept peppering United with questions, asking if the updated plan will increase premiums. In other words, does United plan to cover the losses they’ll see on prescription drugs with an increase in premiums? They told us details are being worked out.
We asked how the change would impact members, when it would happen and, again, whether members will see a premium increase. Again, there was no clear answer from United.
“I think they’re realizing that this is wrong, that there’s a huge liability here, whether fraud or illegal,” says insurance fraud investigator Susan Hayes. “But it’s definitely wrong and I think they realize it.”
Hayes says these changes will only impact some United customers. You may not realize it, but United offers two types of plans to most businesses: one a fully insured plan, the other a self-funded plan. Large companies may take part in a self-funded plan in which the employer pays all of the costs, like part of the copays, and United simply manages the program.
In a fully insured plan, usually for smaller- to mid-size businesses, United takes the risk – it pays the copays and charges the employer a fee. According to the United email and Hayes’ interpretation, the change will only take place for fully insured customers – most likely employees of smaller to mid-size companies.
Hayes tells us United may simply raise premiums on these fully insured plans. She says self-funded plans and customers should be asking United questions.
Read More >>