The upcoming modifications in the Medication Therapy Management (MTM) program by CMS are expected to significantly expand eligibility, with an estimated increase in eligible Medicare beneficiaries from 4.5 million to 11 million. CMS doubles down on medication therapy management (MTM), with program expansion, as self-funded employers remain indifferent to MTM’s vast benefits.
The new eligibility criteria, taking effect in 2025, will include (1) require Part D sponsors to include all core chronic diseases in their targeting criteria, codify the current 9 core chronic diseases in regulation, and add HIV/AIDS for a total of 10 core chronic diseases, (2) lower the maximum number of covered Part D drugs a sponsor may require from 8 to 5 drugs and require sponsors to include all Part D maintenance drugs and (3) revise the cost threshold methodology based on the average annual cost of 5 generic Part D drugs ($1,004 in 2020). These changes are projected to add approximately $336 million annually to plan costs.
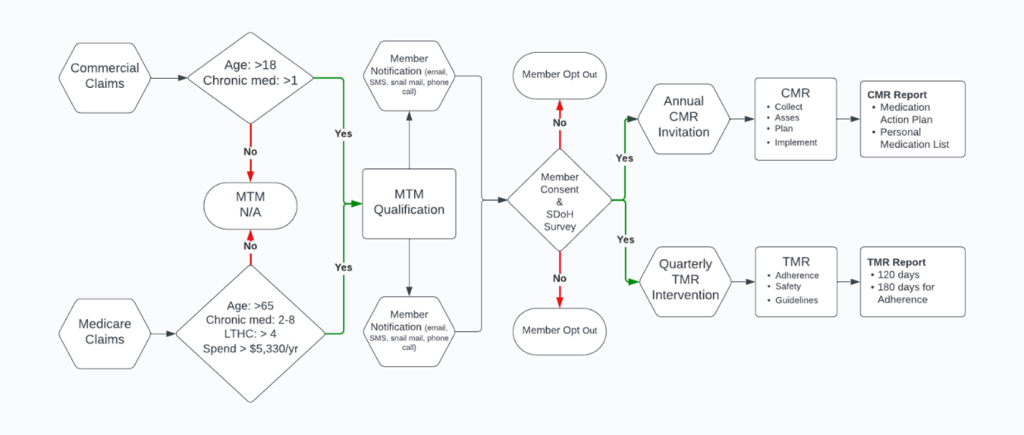
MTM is a key strategy to leverage pharmacy-led initiatives to reduce medical costs. By focusing on identifying and resolving Drug Therapy Problems (DTPs), pharmacists can play a crucial role in conducting comprehensive medication reviews (CMRs), enhancing both health outcomes and cost efficiency. The savings generated can then be reinvested into the MTM program, potentially making it self-sustaining.
The revised MTM guidelines will require Part D plans to include members with up to three chronic conditions, taking at least five Part D drugs, and meeting a lowered annual spending threshold. This will necessitate a more comprehensive approach in CMRs, including real-time consultations through telehealth or in-person visits. To optimize their pharmacy benefit management program, self-funded employers should focus on four main strategies:
- Technological Integration in Pharmacy Workflows: Utilizing platforms that combine medical and pharmacy claims data can help identify a wider range of DTPs, enabling more effective CMRs and facilitating cost reduction.
- Infrastructure Scalability: Evaluating current technology and infrastructure for their ability to handle increased demand and provide scalable solutions is crucial.
- Proactive Member Eligibility Identification: Tools that can predict future eligibility and manage enrollment processes will be essential for efficient MTM service delivery.
- Continuous Program Monitoring: Implementing tools for real-time monitoring and analysis will help in identifying cost-saving opportunities and ensuring the effectiveness of the MTM program.
Self-funded employers would serve themselves extremely well by taking a page from the CMS playbook. By embracing a data-driven approach and focusing on efficiency and scalability, self-funded employers can adopt a CMS-like medication therapy management (MTM) expansion, achieving total cost of care savings and maintaining high-quality service for members with multiple medications and conditions.