Tyson Foods, Employing 140,000, Parts Ways with Major PBM [Weekly Roundup]
Tyson Foods, Employing 140,000, Parts Ways with Major PBM and other notes from around the interweb:
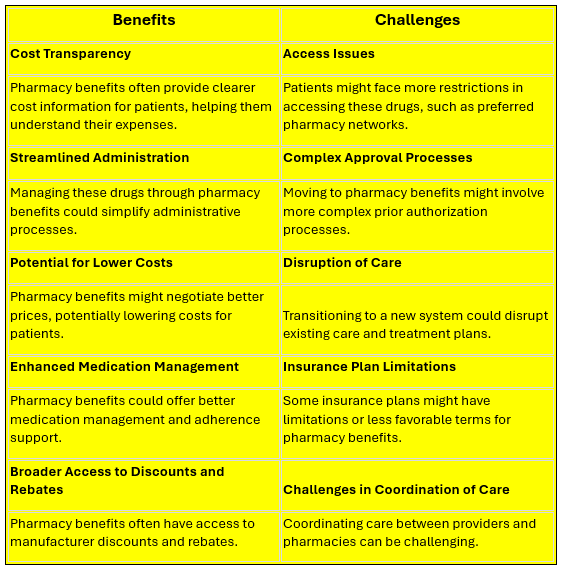
- Tyson Foods, Employing 140,000, Parts Ways with Major PBM. Tyson Foods will become one of the first Fortune 100 companies to stop using the nation’s traditional large pharmacy benefits managers, as it looks to cut spending on high-cost drugs. Tyson’s decision adds to an upheaval in the industry, as startups promising lower costs and transparency challenge the largest benefit managers and pushed them to change their own business models. Tyson made the decision as it saw pharmacy costs soar. “We were going anywhere between 12% to 14% increases for pharmacy — and on a $200 million spend that’s quite a bit. We found that the specialty (drug) component of our trends … were picking up a lot of the increase year over year,” said Renu Chhabra, Tyson vice president and head of global benefits. When she tried to get answers on what was driving those trends from the company’s old pharmacy benefit manger, or PBM, Chhabra says she couldn’t get the kind of data she wanted.
- 5 ways to improve your PBM procurement process in 2024. Many self-funded plan sponsors struggle to manage the cost of pharmacy benefits and rely on non-transparent contract guarantees to hold PBMs accountable. Meanwhile, drug spending continues to compound at an astonishing rate in defiance of the savings promised during the procurement process. As a former pharmacy program director for a plan covering more than 16,000 lives, I can tell you that it is possible to stop the “games” PBMs play, control costs, and ensure that all contractual guarantees are met, especially in scenarios where a PBM won’t guarantee an all-in per member per month (PMPM) cost for the year. Understanding the problem is a part of the solution, but making meaningful changes to the way plan sponsors and brokers evaluate PBMs is where the real opportunity lies.
- 3 thing to know about specialty pharmacy in 2024. Specialty drugs may be covered by a medical benefit (what patient-members likely think of as “their insurance”) or pharmacy benefits. There’s often a gray area for where specialty falls, but it can relate to whether the drug is being administered in a clinical setting, like a doctor’s office, outpatient clinic, or infusion center. Reimbursement for these drugs can also vary between average wholesale price (AWP) for pharmacy reimbursement and average sales price (ASP) for the medical benefit. It’s complex to compare, and both ASP and AWP are used in the health care industry, but they’re different. ASP is a government-regulated tool that uses manufacturer sales information including discounts, such as rebates. AWP is the average price that wholesalers sell drugs to pharmacies, prescribers, and others. A government report found the median percentage difference between ASP and AWP to be 49%.
- Cigna Group to Sell Medicare Businesses to Health Care Service Corporation (HCSC). The Cigna Group today announced that it has entered into a definitive agreement whereby Health Care Service Corporation (HCSC) will acquire The Cigna Group’s Medicare Advantage, Cigna Supplemental Benefits, Medicare Part D and CareAllies businesses, for a total transaction value of approximately $3.7 billion. As part of the transaction, The Cigna Group and HCSC have agreed to enter into a four-year services agreement under which Evernorth Health Services, a subsidiary of The Cigna Group, will continue to provide pharmacy benefit services to the Medicare businesses, effective on closing of the transaction.