Generic Prescription Drugs by Mail can be a Bad Deal
Some simple comparison shopping shows that despite formidable bargaining clout, many employers are paying far higher prices for some drugs than ordinary individuals can get walking into retail pharmacies. Consider the price for Ranitidine 75 mg, the generic form of the popular anti-ulcer medication Zantac.
One of my clients paid Express Scripts $36.22 for 90 pills mailed to a worker, who pays an additional $5 co-pay, bringing the total cost to $41.22, according to a re-pricing we completed. If this same employee had simply walked into their local pharmacy and bought the same Ranitidine prescription it would’ve cost as little as $10.00 for the same 90 pills. This is a 400% difference in cost!
That this employer pays ESI higher prices for many generic drugs than regular pharmacies charge customers without insurance illustrates the complexities, and potential pitfalls, of prescription drug coverage. It’s also a rare glimpse into how such plans work.
Traditional pharmacy benefit managers, such as ESI and CVS/Caremark, administer the drug benefits of large employers, acting as the middlemen between the employers and the pharmacies. Such PBMs create large networks of participating pharmacies and use their size to drive down prescription drug prices.
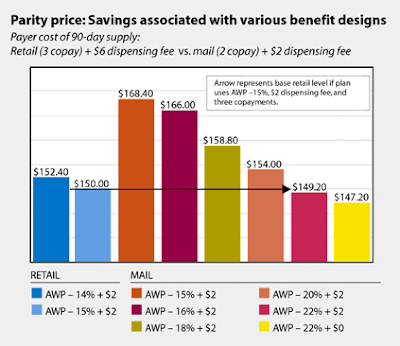 |
| Source: managedcaremag.com |
Some, including ESI and CVS/Caremark, also own their own mail-order pharmacies, and guilt employers to move more of their workers’ prescriptions into the mail business. Traditional PBMs promise to realize savings for their corporate customers by keeping the overall cost of prescription medications down. But, they also preserve large profit margins for themselves, as the above prices clearly indicate.
Some companies say they are satisfied with the overall savings Medco is providing. But others simply aren’t aware of the vast price discrepancies on generic drugs. How can a company say it is satisfied with the overall savings when they don’t even know the actual costs?
Too many companies are spending tens of thousands of dollars on products for which they were never given a price list! These assumed savings are based upon colorful PowerPoint presentations, delivered by PBM account managers, designed to tell you exactly what you want to hear.
Because generic drugs are so cheap to begin with, PBMs and retail pharmacies alike typically make big margins on generic drugs, which account for about half of prescriptions filled in the U.S. That’s why pharmacies have a big incentive to switch prescriptions for branded drugs to their generic versions. Aggressively switching of branded prescriptions to generics does help reduce employers’ drug costs.
Employers also believe they are getting better prices on branded drugs through PBMs, which is why they are willing to pay bigger markups on generic medications. Mail-order pharmacies generally fill a three-month’s supply of medication at once.
Traditional PBMs, like ESI and CVS/Caremark, benefit greatly from its mail-order pricing system. When a patient fills a prescription through the mail pharmacy, the full profit belongs to the PBM, rather than having to split it or get very little when the transaction happens at the retail store.
Some traditional PBMs derive more than half of its corporate profits just from selling generic drugs from its own mail order unit. For example, Ranitidine 75 mg x 30 pills usually cost pharmacies about $2. At retail, customers can pay $10. I’ve seen mail-order prices as high as $181.00! ESI can show its customers a great savings because the list price, called the average wholesale price, quotes Ranitidine at about $214 for 90 pills.
The complex system of drug pricing makes it difficult for employers to know whether they are getting the best prices. Generic drug prices in mail programs are based on average wholesale price, or AWP. AWP is considered an inflated price among those in the drug industry. For example, the average wholesale price for Fluoxetine 20 mg x 100, the generic drug for Prozac, is $240.12 but pharmacies can pay less than $2.00!
Not all mail-order pharmacies are deceptive. A truly transparent mail-order pharmacy, one willing to contractually accept the role of fiduciary, will deliver a significant savings for employers compared to retail. Don’t hire a PBM because of its long history, big offices, or colorful presentations. Hire a PBM because of the value it is contractually willing to deliver its clients. It is really quite simple; if the PBM isn’t willing to sign on as a fiduciary then walk away.
